Ah…the beginning of an article. How to make it click-baity enough to get some eyeballs, yet actually offer value to the reader? Due to old-age or just lack of inspiration I’ve got nothing in this regard, so I’ll get to the story at hand:
A few weeks ago I had a sit-down with the dietetics staff at a medium sized, rural hospital. Super nice folks, very sincere. They deal with a population that is enormously overweight and which suffers from type 2 diabetes and all the related problems. This was a VERY interesting meeting as the folks who OWN the hospital are fully on-board with the Ancestral Health template and are huge advocates of things like the paleo and keto diets. The owners know this stuff works, they wanted to have a sit-down with their dietitians to try to get them on-board with the notion that eating strategies like paleo or keto “might” be helpful for their very sick (and expensive to treat) population. Everyone went around the table giving a bit of a bio and when it came to me I could see the eyes of the poor dietitians grow wide when they learned I’d written some paleo diet books and was a fan of low carb (for the right situations…you know, like fat loss and type 2 diabetes.)
Things got a bit…fidgety after my bio but our moderator did a great job of smoothing things over and asked the dietetics staff to go through what their process is in working with these obese and or type 2 diabetic patients. Again, I do not want to paint these folks as anything other than sincere and well meaning, but here is what they shared:
1-The MAIN item they focus on is getting folks to “drink more water.” This was mentioned and reiterated at least a dozen times.
2-Their avant garde initiative was to have families eat together, but a point was made that they “should not in any way criticize or second guess what they were eating” and yes, that IS a direct quote.
I want to unpack the second point first: I cannot think of a better basic recommendation that families should share meals together. Life is short, family is everything. Turning off the TV, putting away the smart-phones and other distractions and “talking” is a lost art these days.
THAT is awesome.
But…
In what was at least a 15 minute presentation, food-quality was not mentioned once. And upon inspection of the literature which supports this program, the claim was made that this mindful family eating was THE route to reversing weight and health issues that are dietary in nature.
Community IS one of the four pillars of health (along with sleep, movement and….food) but what was related to me is the vast majority of meals taken by these families were fast food, desserts, and what would generally be termed “highly processed snacks.”
Now, I do think far too much emphasis is placed on “diet.” For example, most people citing the upsides of Blue Zones focus almost exclusively on diet and pay little attention to the extended communities which are clearly a major factor in the health and well-being of these populations.
But the folks in the Blue Zones are NOT eating fast food. Ever. Not yet.
I asked these folks how they felt the program was working…as in, did they see decreasing rates of death and disease, were medical costs going down. These folks mentioned “evidence based medicine” quite frequently and I asked what one would consider to be a reasonable question about the efficacy (evidence of results) of this mindful-eating initiative. What I got was a pretty defensive back-pedaling as the unfortunate reality is the costs of dealing with all these diet and lifestyle related problems has continued its upward trend, which by the way is exponential in nature (understanding the implications of exponentials in this scenario might be worth unpacking in a future article.)
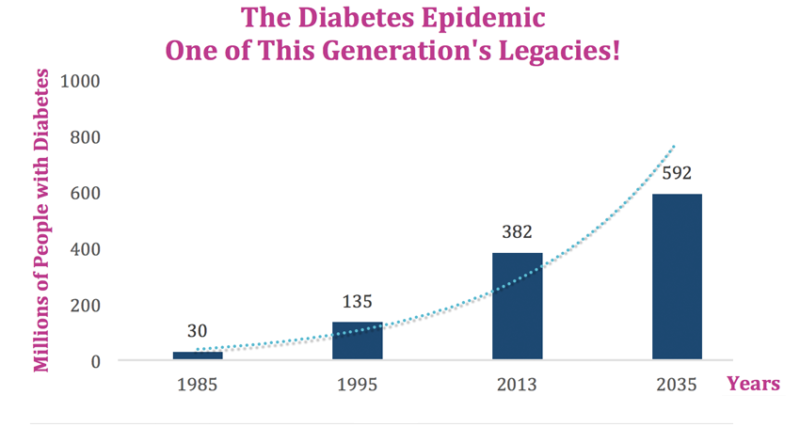
So, despite good intentions, this mindful eating program is not producing results that really matter.
You may think I’m being a big meanie here, but I’ll share an example of how this thinking is failing the population these folks are entrusted to serve. I asked for an example of one of their most challenging and expensive situations. This turned out to be a middle-aged male who is type 2 diabetic, on dialysis and he is now effectively a trunk. ONLY a trunk. Both arms have been amputated at the shoulder, both legs amputated at the hips, all due to diabetic complications. This poor guy has suffered a slew of surgeries (those limbs come off in pieces, not at once…toes, then foot, then lower leg…you get the picture) and must be medically transported multiple times per week for dialysis…then you have his medication costs and the fact he is no longer able to work and needs a full-time care provider. I won’t even relate how much this one individual has cost this system (and continues to cost) as you’d think I’m making the number up.
Fifty years ago this scenario was UNHEARD of. It did not happen. It is now commonplace…and the best “evidence based medicine” recommendations these healthcare providers can offer is “mindful eating” and an insistence that folks should not worry about their food quality. They do not want people to feel shame about what’s on their plate. Before you are Triggered and put words in my mouth, I am not advocating these people should be shamed in any way. But I do think this is an epic failure on the part of the folks tasked to educate and help these folks. Pushing for food quality is the only way this story is going to change and even doing that is going to be tough to implement when we consider the nature of our modern, hectic lives and hyper-palatable foods. Our best efforts are likely to produce lackluster results, but this is not remotely our “best efforts.”
Ok, now to point #1 from above: Drink more water.
These folks were absolutely starry eyed at this suggestion, and they did say they have seen improvements in this area. Often, “water” is interpreted as “soft-drinks” but to the point above, there is a nervousness around suggesting there may be better and worse options as it might make someone feel bad to suggest sodas, although tasty, may not be all that healthy. I asked these folks what they felt, from a medical and physiological perspective, drinking more water would do for folks.
The responses fell into two camps:
1-People are “chronically dehydrated” and this is a major health concern.
2-Drinking water “fills people up.”
To point #2 I will simply say “no, drinking more water does not cause people to spontaneously reduce caloric intake.” I’ll let you practice your Google-fu in digging up the citations on that. On point #1 I’ll refer you to this article and pull out a few highlights on heat related deaths/illness, particularly in athletic populations. Why am I using this information? People who are active tend to require more water. People in warm settings require more water. So, exercising in the heat….man, we should really see the dangerous effects of dehydration, right? Well, from the article:
The Myths of Dehydration and Heat Illnesses
- -The primary cause of hyponatremia in athletes is drinking too much water.
- -The incidence of hyponatremia appears to be between 13% and 15% among endurance athletes.
-Sodium supplementation has no effect on the occurrence of hyponatremia. - –There seems to not be a single case of death resulting from sports-related dehydration in the medical literature.
I bolded that last line and I should mention that hyponatremia is low blood salt…which is usually accomplished by consuming too much water, not too little salt.
Now, each year there are a not insignificant number of deaths/hospitalizations in the military, sporting events, hiking etc, and it is absolutely related to water…but it is generally due to TOO MUCH. I looked and looked, and what I consistently come back with is that last bolded line: One is hard pressed to find ANY examples of people dying from dehydration, even in remarkably challenging settings. People do not die and in fact do not become ill due to dehydration in the most extreme of physical activities, even in the heat…so how can one make “drink more water” the go-to recommendation for a sedentary population that spends an inordinate amount of time indoors, under near perfect temperature control?
About 700 people die each year in the US due to heat stroke. These tend to be infants, the elderly and the obese. These are populations with impaired ability to sweat and regulate body temperature. I’m not making light of that, nor am I saying that is not an important issue, but what I am saying is the focus on “drink more water” does not really address the challenges in these heat stroke examples, and appear to be not only be unhelpful, but injurious to the general athletic population.
How did this meeting wrap up? I cannot say it was a “high note.” We agreed to flesh out some common goals of educating folks about “eat whole foods” but even this seemingly benign angle on my part was met with near panic on the part of the dietetics staff.
There is a remarkable amount of energy being put into various healthcare debates, particularly in the US. These debates focus mainly on “who is going to pay” with some advocating for a system like auto insurance in which one largely pays as one goes and has a catastrophic plan for accidents, vs something folks familiar with the NHS, Canadian or Northern European models would be familiar with. I do think it’s important how we set up incentives in situations like this, but debating about who will pay for a system in which the costs of dealing with diabesity related problems are increasing exponentially and are on track to bankrupt the developed world is at best rearranging deck-chairs on the Titanic.
I will release an article on exponential costs in a week or two to provide some context here.
We face an incredibly complex problem of having a set of genetics wired for a different time, and a modern industrial food system that is a master at producing what is effectively addictive, hyper-palatable food.
If I could wave a magic wand and have every healthcare provider on the planet fully bought-in on the ancestral health model, if all these folks recognized a low carb diet can work miracles for diabesity…we’d STILL have a monumental challenge ahead of us.
We have none of that.
We have gate-keepers that are afraid to tell people “food quality matters” and the best our healthcare providers have to offer (drink more water) appears to be at best a waste of time, at worst, it may be making the problem worse.
What to do?
When I think about this two terms keep coming up: Grassroots, Trench Warfare. Grassroots means we are unlikely to see effective solutions offered up from on-high. There is too much money, inertia, ego and confusion in the dominant paradigm to just do an about-face. Grassroots means starting locally and this is where we transition to Trench Warfare: We gain ground anywhere the opportunity arises.
Although information is not generally THE thing that makes people enact significant change, if we do not have at least decent information, it’s tough to get things oriented in a way that we have any hope of success. “Drink more water” is not going to cut it. Where Grassroots meets Trench Warfare is the growing number of health practitioners who are steeped in this Ancestral Health/functional medicine model. If you’d like to learn more about this movement check out my podcast with Chris Kresser as we talk about his recently released book, Unconventional Medicine.

Generally love Robb’s material. Think he missed the mark on the hydration thing. But possibly only due to semantics. Patients who are sedentary and in climate controlled environments will benefit on a cellular level (ie. Signaling) from being properly hydrated. Only hydrating with actual water rather than increasing hydration by way of soft drinks and juice seems like a message hidden within this article but not teased out.
Well amigo, this is a bit of art imitating life, or some kind of fractal thingy: I look at all elements of the hydration piece of this story as a dripping faucet. I see the rest of the story as a fully involved house fire…with that dripping faucet inside. Yes, addressing the dripping faucet might be good at some point, but that fire that will bring things to the ground…THAT should get a bit more attention!
I beat Diabetes 2. The American Diabetes Association informed me, “Once a diabetic, always a diabetic”. So did Humana. Wrong, wrong, wrong. My primary care doc says I am “totally” out of the diabetic range. My AIC is 5.4. I was diabetic 8 months, 12 units of insulin, twice daily. I am also 100% disabled, cannot exercise normally. I have been diabetes free two years and no pills either.
It can be beat. Yes, I’ve heard the water thing over and over. BS. Lower carbs. Weight and calories count. Test your sugar daily and after meals to see what works and does not. I did it on a low budget plan. You can too!
I’ve had many discussions with registered dietitians and I’ve come to a few conclusions. When they first enter school they have an operation on their brain and their common sense is removed. I too have seen the starry eyed look they get as if they are off in a world to their own.
You cannot combat type 2 diabetes with the amount of carbohydrates that the FDA Dietary Guidelines recommend. It not only has never worked but it makes matters worse.
I only work with client who really want to be diabetes free and I am a ketogenic LCHF advocate. It works, when the client follows the program. Not only are they off their medications and diabetes free, but all their numbers, blood pressure, LDL, HDL and triglycerides improve. Why won’t the FDA see this?
Biochemistry fan!
Practical applications to real life in a world of creativity and freedom.
Hi Robb,
I’m not sure what it’s like in the US but in the UK eating healthy (organic, grass fed) is expensive. The average working class family (I hate to pigeon-hole, but this is where the majority of diabesity cases sit) can feed themselves for a week on high carb ready meals for the price of one basket of wholefoods.
Do you think there is scope for govt subsidising healthy eating rather than the health services?
Tom
First I’d scrap subsidies that lead to junk food, then I’d try to find some incentives before the subsidies…but yea, that could be an option.
I’m certainly NOT advocating for forcing chronic hunger and malnutrition on the wielding class and poor, but generally speaking, reallocating those food dollars to higher quality and less quantity is probably in our own best interest. In other words, I can offset the increased cost by buying five days of high quality food instead of seven days worth of low quality food, which in a population suffering from obesity and diabetes should be a double win (increased food quality and a decrease in calories, both of which are needed), but obviously requires a HUGE shift in mindset.
I find it crazy that dietitians aren’t talking about good quality and a balanced plate. Even the USDA food plate model would bring carbs somewhat down. I am a dietitian and I work in an urban hospital with mostly low income patients. While I absolutely come from a whole foods/Paleo -ish slant, with most people it is mostly starting from eating fewer refined carbs, ditching soda, increasing protein and veggies. I am actually surprised when I have a patient to whom I don’t say some version of eat fewer carbs to. Now whether patients comply is a completely separate issue. Glad you are helping them, though typically dietitians do not trust non dietitians for nutrition info. Maybe you should take Amy with you next time 😉 nice work as always Robb.
My husband recently had a conversation with an acquaintance who is a diabetes educator at one of the top five ranked hospitals in the US. She acknowledged to him that low-carb can work for diabetes control but people just can’t eat that way. Can’t, not won’t. Which makes me think that she’s not even presenting patients with the idea that they could have a little bit of agency in their lives by paying attention to their diet. So, what is she educating them on, what gangrene smells like?
The wacky thing here is “they” told “us” to eat less fat, and we have generally done that. Why a suggestion of fewer carbs is un-doable is beyond me and even if adherence is low, do we tell the truth or just lie to these people??
If these dietitians aren’t recommending more fruits and veggies and at least lean meats, then they aren’t even remotely close to the U.S. dietary recommendations (inadequate as they are), which should be the standard they’re going by with that bullshit claim of “evidence-based medicine.” I wonder why they think that advising people what to eat is the same as shaming them? I’m an RN and have said a great many things to people about their lifestyle through better food and exercise. Frankly, so long as we phrase things politely and respectfully, we don’t need to worry about people thinking they’re being shamed.
IDK Jennifer, but they were adamant that there be no qualitative commentary on the food.
You’d be surprised how many americans don’t drink any water. A lot of their patients may only hydrate on soft drinks, coffee, etc… Probably the reason they stress drinking water so much. Sounds like they don’t want to judge diets/lifestyle and saying drink more water is probably the passive/PC way for them to try to cut down the crazy amount of sugar/chemicals etc… these people drink everyday (and drink some real water)
I especially enjoy when you link the nutrition to policy and conversation with the status quo. Thanks for this.
I agree completely with Robb. As a long time listener/reader, I give him major props for staying consistently on message about this for years and years without giving up. Where he is the most spot on is in the Grassroots/trench warfare recommendation. If we could crowdsource some kind of template that would allow regular, non-healthcare affiliates joes and janes (like me) to start to establish local, grassroots efforts to educate and empower our communities to make better health and lifestyle choices, maybe there is something we can do. I hesitate to suggest looking at how religious/faith-based orgs set up shop in communities for an example of how a grassroots health and lifestyle education org might do the same, but some of the same ideas may be worth adopting?
Thank you!!
it is interesting how traditional diets and returning to family, building community, and, hey, perhaps contact with God, might lighten up efficacy of the slow kill of the cash cow of the medical mafia (Americans who follow suggestions of the FDA, CDC, AMA, etc). Culturally we left the country for “opportunity” in cities, started eating junk food for expediency, stayed away from creepy religions because of its obvious flaws…and then, here we are! I admire your ongoing diplomacy especially when in the belly of the beast, Robb!
Well, as a diabetic,i not taking medicine, alot of water and re vese my diet. Dolng great. Thank you.
I live in the uk and obesity is rising all the time so I agree with Rob but I don’t see why you have to dress the message up for fear of offending people, it’s for the good of their health. Just say eat less carbs and processed food then list the foods high in carbs ie white bread, cakes, doughnuts, biscuits etc. When I was a single parent with four children and not much money we ate fresh vegetables, often in the form of soups and stews where a little meat goes a long way and fruit instead of high carb puddings so I don’t agree that a healthy diet is more expensive, it just means that you have to cook – using raw ingredients – there’s a radical thought! I do think people need cookery lessons, people used to learn either from their mothers or at school but as it was only the girls who learned to cook it was deemed sexist and stopped, instead of just including boys. Another important point is cut out snacking and never eat unless sitting at a table and never eat in the street. If I were in government I’d ban eating in the street, thereby cutting both litter and obesity in one go!
I am in total an utter disbelief at the ignorance of these so called health care providers. It’s one thing that the dieticians may be operating from old information from when they were in school and a completely other thing that they obviously haven’t applied their mind in looking into the mainstream research which completely validates the Paleo/Ancestral lifestyle. Hopefully they’re not still recommending margarine!
I always find it weird that families don’t sit down and eat meals together. My family has always done it everyday! Even if we weren’t all eating the same thing we would all time it to be at the same time.
The research that comes up on google, mostly observational but also a few, mostly small n, trails, seems, at least after a brief skimming, consistent with the notion that getting people to drink more water may lead to greater weight loss. New to this blog, so I realize that I may be ignorant of some standard responses to these lines of evidence/argument.
Things found via google:
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2929932
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2859815/
https://www.ncbi.nlm.nih.gov/pubmed/26537940
I would like to point out that it would definitely lead to weight loss if they switched from drinking soda and fruit juices to water, because they’re cutting out a lot of calories. That in itself will lead to weight loss.
Stuff like this makes my head want to explode. Yes, drinking more water is great if it is replacing sugary drinks. Yes, sitting together and eating mindfully is great on so many levels. But they should be shouting “STOP EATING CRAP” from the rooftops. And then let them know what the crap is.
Hallelujah! It’s all the junk that people have been eating all these years that’s been causing this diabesity problem!
Great article and maddening for all the reasons already commented on. My question is about hydration. Can you offer some reasons that I often feel thirsty even after drinking anywhere from half to a full gallon of water throughout the day? I eat plenty of salt, too, so I doubt I’m in danger of throwing off the balance. Though I may crave salt so much because of the amount of water I drink?
I have the same problem. I’m not exactly on a Paleo diet, but more of a keto diet, and I’ve been told that when you’re in ketosis your likely to get very thirsty. This is supposed to be temporary, but with me that symptom has never gone away.
Have you tried adding in electrolytes?
Just quite in time article for Holidays Robb. I do believe in you man.
I personally get started about 2 months ago with Paleo and already feel amazing . I did it all thanks to the help of a book series that my friend Max told me about I am sure this will provide treendous value to anyone that sees this.
if you want you can check it out here: https://tinyurl.com/ycelj2gj
Robb, I am curious about the “near panic” state among the dietitians at the end of your meeting. Would you ascribe this to industry professional pressure (eg, climate of “we don’t question diet…or else”) or simple reluctance to put their patients on the spot? Possibly lack of expertise? (although…they ARE dietitians…) Could you tell? Thanks for the thought provoking material.
Prof Tim Noakes wrote a book called Waterlogged that is worth reading. In short it supports Robs view in water.
I hear what you are saying but according to IHRSA only 19% of the population works out, maybe less. So 81% of the population is not and does have dehydration issues. Ive been an Active Release Techniques provider for 19 years. Ive studied under Dr Michael Leahy (ART) , French Osteopath Dr Guy Voyer, Tom Myers of Anatomy Trains, Dr Eric Serrano and Dr Jeffrey Morrison (NYC). They will all agree there are a lot of dehydrated people out there in the general public. I know many body workers who see this on a daily basis. The top athletes , usually, not always eat well and drink water. But its a small % of the population.
I am surprised by how much emphasis in the article, and some of the comments, is placed on not wanting to communicate a hard message to people about food choice. It is not about shaming, it is about telling the truth. Only when people are fully aware of the truth can they make a conscious decision about their choices and the implications. The entire concept of trying to be PC and not send the hard messages while people are suffering and costs are rising out of control is insane. Robb – keep spreading the word and don’t hold back. People need to hear it loud and clear.
Robb,
Great piece. I am not surprised at all at the RD’s responses. Conventional medicine is just now being FORCED to realize that diet matters, but food quality is so out of their scope of understanding. I mention to colleagues in Pediatrics, who give me similar response. In trying to not make a mother feel bad about what she feeds her child, we don’t mention the foods (and quality of) which she should give. Then in order to justify the advice (or lack there of) the existence of any evidence is denied. We have a lot of work to do.
Two things to add to this discussion.
1. When I have gone on a hydration regimen I have found that the water goes in one end and comes out the other. I actually feel thirstier after “hydrating” for several days probably because electrolytes are being washed out of my body.
2. Those of us living in urban areas are hardly drinking what you could call pure water. When municipalities added chloramine to the chemical cocktail of fluoride and chlorine I developed gastric intestinal problems. It took me quite awhile to figure out tap water was making me sick. But the overwelhimg evidence was there. Why would so many people start buying water in bottles if not because of a gut feeling like mine literally. On the heels of the Paleo diet now comes the gut biome rediscovery and the need not to kill off our beneficial bacteria with chemical laced water designed to kill bacteria .
The missing information here is what is the minimum quantity of daily water intake for a “normal” person (or shades of normal persons based on phisical activity) to stay out of dehydration, and what is the mark above which water intake becomes counter-productive or damaging…
Oh Robb, this is precisely why I can’t work in the field that I got my degree in. As a therapist in rehab centers, about 85% of my patients are there due to lifestyle choices: smoking, alcohol, obesity, sedentary lifestyle, poor food choices,etc. Imagine having to enter the room of a 550 pound bed ridden patient armed with nothing but a pep talk and 3 pound dumbbells. It’s just so depressing. Then you glance the room and it’s stockpiled with cans of grape soda, cigarettes, and pizza boxes. Bariatric beds and wheelchairs are the norm. Some of these old rehab centers need to be remodeled because their doorways aren’t wide enough, and their toilets won’t support a 400 pound person. The halls are littered with Hoyer lifts and the kitchen keeps sending out meatloaf, “healthy grains,” salads with fat free dressing and little packets of “Mrs. Dash.” Water is — literally— a drop in the bucket.
Wow Robb, I’m not sure how you make it through a meeting like that-over and over again! But thanks for doing it. I went for a blood draw from Quest Diagnostics that is now located in Safeway and as my sweet but obese phlebotomist made the draw, I thought how ironic that I have to walk through the cause (salad dressing aisle) to measure the effects. Hmmmm…
I would like to add my thoughts here. It does cost more money for healthy food than it does for junk. However, when eating paleo / Keto, one generally eats less food, so that pretty much offsets the cost. I generally eat only two meals a day, because I’m not hungry enough to eat three. It does cost a lot more for grass-fed meat and organic foods, and I cannot afford to buy that all the time. I think the best thing is for people to just stay away from processed foods and eat everything in its natural state, cooked or raw. I know some people advocate eating only raw foods, but I prefer most of my food cooked. It is difficult to get people on a lower income to eat right. Many of them are going to food banks for their food. Been there, done that! Most what you get at food banks is processed junk. Stuff that no one should be eating. They don’t give out enough fresh veggies and meats. A lot of canned foods, breads, junky snacks, etc. until this changes, I think those on a low income are going to find it very difficult to eat healthy. And it certainly doesn’t help that the u.s. government food pyramid tells us to eat most of our diet as carbs. I think a lot of it has to do with big Pharma wanting people to stay on their medications, because they stand to lose a lot of money if everyone gets healthy.
Robb –
I’m totally down with your advice on all things and credit the Paleo Solution with opening my eyes to a new healthful way of living. Some time ago – possibly following the bad advice you mention in your piece – I started to drink more water deliberately. I target half my body weight in ounces daily, though I often exceed that amount. Apart from black coffee, water is all I drink. Here’s the thing: I feel really good when I hydrate that much.
If it works well for you, then go with it.
The diabetic education in this country blows me away! I have clients repeatedly bring me the “dietary guidelines” that they are told to follow as a diabetic, and they recommend foods that we know CONTRIBUTE to metabolic chaos in the system! To tell people to consume artificial sweeteners, fat-free foods, etc is completely absurd!
What’s cool is, our team has just been approved to be possibly the first non-medical, health insurance fully-reimbursable approach to reversing diabetes. It’s a pilot program that the insurance company is covering 100%, knowing fully that we will be coming from a completely different approach than the standard of care currently being taught to new diabetics.
The point is, they know the old way is NOT working, and it’s time to step up and give patients the tools to truly reduce/eliminate their costly dependence on pharmaceuticals.
My son started university ten years ago as a pre-med student. The school he attended offered one of several disciplines as a choice for “pre-med” so he chose “nutrition.” He loved his science classes, which were taught by professors who were researchers themselves and excited about the breakthroughs they were regularly seeing, and the cooking classes, taught by professors who were actually up-to-date with the research. (In one class he baked a pie using lard as the fat for the crust – it was not only presented as the “healthiest” option but touted as producing the best results. My Grannie would have agreed.) But when he got to the actual “nutrition” classes, the ones taught by the “Nutritionists” who had worked for hospitals and written policy papers, he became frustrated and disgusted. Not one was aware of any science that challenged their dogma, much less willing to listen to any student who, coming straight from those exciting chemistry courses, dared to offer up data that would overturn the course truisms. During finals his next-to-last semester he called home despondent: he knew that if he didn’t get accepted into med school he’d only be qualified to go to work as a “nutritionist.” He was horrified at that prospect. He switched majors and eventually graduated with a degree in business, and now finds himself giving his friends and co-workers (and sometimes even customers) nutrition and fitness advice. He recently finished a certain Paleo guru’s certification course in order to have some letters next to his name so that he’s a bonafide “expert.” He has confided that the only students he knows from that nutrition program who went on to become “nutritionists” were the ones he’d never been impressed with academically. He regularly tells people that the academic field of “nutrition” is a farce and that if they want to take charge of their health they must throw out almost everything “official” and turn inside out the knowledge they’ve absorbed through any mainstream source. People who listen to him get results and refer their friends. He’s a grassroots source of trench warfare. His education experience is also instructive as to what we’re up against.
that’s rough!