It’s funny how our mental state really affects how we write and what we are interested in. When I wrote the introduction to this piece I was just getting settled into our new place in Santa Fe, NM and was looking at over a month at home to work and write. Then a number of wacky events happened and I’ve been home about 7 days out of the last month and I’ve only made it about 70 pages into Kon-Tiki.
Ouch.
Now I’m home for 8 days and will then be gone for a project that will take me completely off the grid for nearly 3 weeks. No phone, email…nada. When I sat down to do this kidney piece it was with a mindset that I had a ton of time and could really sink my teeth into it. Now I’m time crunched and anxious that I will get it done at all! Up front here I’d like to thank Mat “The Kraken” Lalonde with his help on some literature for this piece. Any inaccuracies however are my own tomfoolery.
If I wanted to cut to the chase I could boil this whole thing down to the following:
1-Dietary protein DOES NOT CAUSE KIDNEY DAMAGE.
2-Chronically elevated BLOOD GLUCOSE levels DO cause kidney damage.
3-Dietary fructose REALLY causes kidney damage.
4-Many kidney issues have either a hyperinsulinemic characteristic, an autoimmune characteristic, and or a combination of autoimmunity or hyperinsulinism. A standard, low-ish carb paleo diet can fix most of these issues.
5-For serious kidney damage a low-protein, ketogenic diet can be remarkably therapeutic.
6-If you get kidney stones that are from oxalates, reduce your green veggie intake (spinach for example) and have other types of veggies.
7-If you get kidney stones that are from urate salts, you are likely NOT following a low-ish carb paleo diet, you likely have insulin resistance and your liver is not processing uric acid.
As much as I’d like to leave it at that I’d be asking folks to operate on faith, not facts, so we need to do a little more digging. First we’ll look at normal kidney function, some common renal pathologies, how one might go about fixing those pathologies, then a clinical note or two.
Renal Function
The kidneys control a remarkable number of biological parameters, at least in those critters with kidneys! This includes blood pressure, filtering and removal of various metabolic waste products, blood volume, red blood cell count, electrolytes, acid base balance…Guyton’s Textbook of Medical Physiology has nearly 200 pages devoted to renal function, and that is a bare-bones overview with little time spent on pathophysiology. The lions share of kidney function involves filtration of the blood via a counter current exchange process that biology makes use of not only in kidneys, but also in the distal portion of limbs. In the case of kidneys, the counter current process retains or excretes various dissolved items as needed. In the case of limbs it’s an efficient method of minimizing heat loss (this is a common feature of the feet of birds who spend time with their feet in cold water).
Renal function is generally measured by glomerular filtration rate (GFR), but other indices are helpful including blood urea nitrogen (BUN) and the presence or absence of the protein albumin in the urine. GFR, when properly interpreted or implemented, should tell us how much actual filtration is occurring in the kidneys. If we know the concentration of an item like creatinine (a by-product of creatine breakdown) in the plasma and in the urine, then we have a good idea of GFR. The problem with creatinine is folks with larger muscle mass, or who train hard can have seemingly elevated creatinine levels, which can make GFR appear to be low. This is why it’s smart to also consider BUN and albumin. If BUN is going up we know the kidneys are NOT doing an adequate job. We are after all, accumulating nitrogenous waste products in the BLOOD (blood urea nitrogen). Conversely, if we see elevated albumin in the URINE we know we likely have kidney damage…proteins that otherwise stay in the blood are getting pushed into the glomerular filtrate (urine). In situations such as blood sugar highs in diabetics we can see glucose in the urine as a coping mechanism to bring blood glucose levels down, but that situation is bad, bad business.
Here is a brief recap of that:
1-Increased Creatinine: May not mean much, NOT a bullet proof demonstration of GFR.
2-Increased BUN: Bad news. GFR may actually be low, we are accumulating toxic nitrogen breakdown products like a boat taking on water.
3-Increased urine albumin: No Bueno. The kidneys are damaged, protein that should stay in the vascular system is leaking into the urine.
4-Glucose in the urine: Five Alarm No Bueno. As we will see, diabetes and the peri-diabetic state is hell on the kidneys.
Basic Pathophysiology
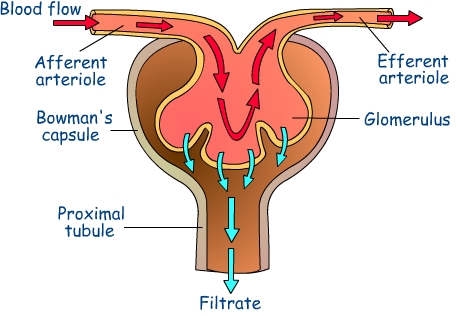
Before we get all pathological, let’s first consider the basic units of the filtration system in the kidney:
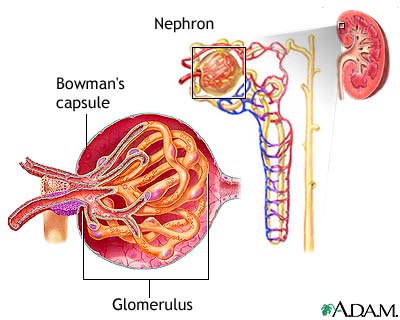
In the first photo we have the Glomerlus which is neighbored by the the Bowman’s Capsule. The glomerulus itself is comprised by the afferent blood supply (in) efferent blood supply (out) filtration surface (kinda like a coffee filter) and the beginning of the proximal tubule (the coffee pot). This is the first stage of filtration in which large amounts of the fluid portion of the blood are literally pushed through the glomerlus and accumulate in the proximal tubule. In the second photo we see not just the Bowman’s capsule and glomerlus, but the whole functional unit of the kidney, including the distal tubule, loops of Henle etc. If you notice this structure is wrapped in a vascular web and it is at this interface that we can create either a dilute or concentrated urine depending on if our hormonal system is actively transporting things like sodium into the filtrate, or reabsorbing sodium (or other solutes such are urea) back into circulation.
As we will see, kidney function can head south from a variety of causes, but we will also see how our modern diet and lifestyle can compound pathogenic factors that bode poorly if you are interested in dead sexy kidney function (DSKF).
Physical damage
I’m not going to look at impact injury or trauma per se, but just keep in mind much of what I’ll describe below applies to trauma for the simple fact it damages the structural elements of the nephron. When I was Thai boxing many years ago I took several very nasty knees to the low back…and had blood in the urine for several days as a consequence. Some motocross riders experience the same things simply from the jarring of landing jumps. Many of our modern activities are damn fun, but not the healthiest of things to do!
When we consider how delicate the nephron is it should not be surprising that damage to various elements can cause problems. The main modes of action we’ll consider are advanced glycation end products (AGE’s), inflammation, abnormal growth, autoimmunity and hormonal alterations affecting kidney function.
AGE’s
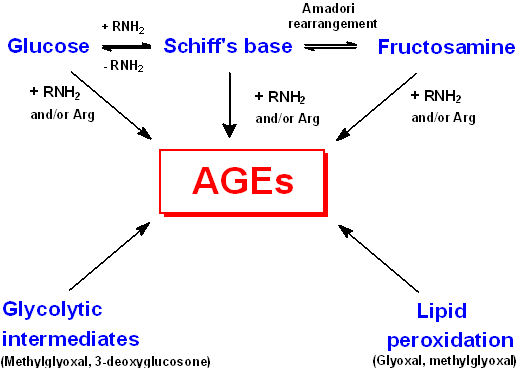
You’d need to be living on a desert island to not know about AGE’s and their potential to negatively affect health. As the name implies, glycation is a process whereby a sugar binds to a protein or lipid. Now, this can happen enzymatically in the case of glycoproteins and glycolipids (a nifty way to modify the structure of these molecules and subsequently their functionality…this is also a major feature of immune recognition) or non-enzymatically, which is what we will look at. Free glucose, can, will and does stick to various proteins and lipids in our bodies via this non-enzymatic process. This is not a good scenario, as it does change the FUNCTIONALITY of these affected structures. Fortunately, we have enzymes that work to undo these unscheduled glycation events, and things work pretty well if we keep food and lifestyle within certain tolerances. In the case of metabolic derangement we have chronically elevated blood glucose levels which drive AGE formation in a concentration dependant fashion: more glucose means more AGE’s, and this can reach a level that overwhelms the enzymes which work to undo the AGE’s. Then we have fructose. Fructose has several unfortunate characteristics:
1-It tends to be processed mainly by the liver, so it’s tough to get it out of circulation.
2-Fructose tends to alter liver function, contributing to insulin resistance.
3-Fructose is structurally more reactive than glucose. At any given concentration, we can expect fructose to produce more AGE’s relative to glucose.
4-Fructose tends to be pro-inflammatory via actions on both the liver, and alterations in gut bacteria.
AGE’s are problematic for kidney function as they damage delicate structures such as the glomerlus, which can limit normal GFR. Damage to the distal portions of the nephron can alter reabsorption. The net result is that our ability to filter out toxic substances such as urea and or regulate normal fluid and electrolyte balance are dramatically altered.
Inflammation
As y’all know, inflammation is a normal process caused by elements of our immune system. Normally this protects us from bacteria, viruses, parasites and cancer, but abnormal amounts of inflammation can get us in hot water (urine?). This is an interesting paper which demonstrates fructose is problematic for kidney function and one of the modes of action is actually an increase in inflammation via increased monocyte chemoattractant protein-1 (MCP-1). Monocytes are part of the innate immune response which we now understand is at ground zero in metabolic derangement and overall systemic inflammation. Once one element of the immune system is on alert, things tend to spiral out of control. In this specific situation, monocytes attack elements of the nephron, causing damage and decreasing renal function. Which leads us to…
Autoimmunity
Autoimmunity is when the adaptive immune system (the wiley part of the immune system responsible for producing antibodies…essentially a remarkable type of information processing and “memory”) begins to attack the host. Well known forms of autoimmunity include rheumatoid arthritis, multiple sclerosis and lupus. Less well known autoimmune diseases that affect the kidneys include autoimmune glomerular nephritis, which is actually a form of systemic Lupus. If you have attended either my seminar or Mat “The Krakn” Lalonde’s seminar, you will know that autoimmunity appears to have features of intestinal permeability with specific autoimmunity being driven in large part by genetic factors. Not surprisingly, a little investigation into search terms such as “glomerular nephritis + gluten” or “glomerular nephritis + trans glutaminase” produces some VERY interesting returns. If you need a reminder about the role of transglutaminase in autoimmune disease, please read this review on celiac disease a model for autoimmunity.
Hormonal factors
Hyperinsulinsim
Chronically elevated insulin levels appear to have a number of causes (excess fructose, linoleic acid (n-6), sedentism, inflammation, sleep disturbances…) and a shocking number of consequences. Most common are Type 2 diabetes and obesity, but linkage to hyperinsulinim includes various types of cancer, mental decline, acne and renal problems for a short list. In the hyperinsulinemic state we have several problems we have already visited (AGE’s & inflammation) but have another interesting wrinkle: elevated growth factors. During the hyperinsulinemic state liver metabolism is, well, broken. We see a decrease in the production of sex hormone binding protein (SHBP) which can be a growth promoter, but we also see an increase in various growth factors including epithelial growth factor (EGF) which can be problematic for a number of skin conditions, and vascular endothelial growth factor (VEGF), which, (you guessed it) can damage kidney function. The structures of the nephron are literally only a few cells think at best. If these structures become damaged due to inflammation, or thickened due to abnormal growth…the system will fail. This study shows how powerful the removal of excess VEGF can be in a diabetic mouse model. The long and short is that even with the other complications associated with diabetes (AGE’s and increased inflammation) the removal of VEGF dramatically improved kidney function.
Aldosterone
Aldosterone is a critical hormone in regulating electrolyte balance, total blood volume and blood pressure. The action of aldosterone is to cause sodium retention and potassium excretion, with the net effect being an increased blood volume. Hyperinsulinism causes increased blood volume as aldosterone production is increased in lock-step with insulin production.
Cortisol
Cortisol has similar effects to aldosterone (sodium retention) but is much less potent in this regard.
Hormonal Effects of sleep
This could be a long post unto itself, but I’d like to look at the action of sleep deprivation on aldosterone. Interestingly, sleep deprivation blocks the nighttime pulsitile release of aldosterone with an interesting effect…of increasing nighttime urine production. Elevated cortisol & hyperinsulinism both alter normal sleep cycles, and have as clinical manifestations, increased nighttime urine production. Which further disturbs sleep, buggaring insulin sensitivity and increasing cortisol levels. You could look at it like this: Hyperinsulinism causes us to retain sodium and water, but also tends to disturb sleep. this alters normal nighttime aldosterone production…causing the frequent trips to the privy at night.
Hey Robb! What about protein and kidneys?
Hmm…how to tackle this tactfully. In healthy kidneys protein intake has NO EFFECT on kidney health. In sick kidneys, protein can cause problems. Why? Because when the kidneys are not excreting urea bad things happen. Urea itself is not particularly toxic, but other nitrogenous waste products are neurotoxic and can cause death at high enough levels. The bottom line is that in healthy individuals, increased protein intake causes an increase in the kidneys ability to deal with creatinine and BUN. In individuals with kidney disease they will likely benefit from a decrease in protein intake…but they need to address one of the aforementioned factors if they want to REGAIN kidney function, which we will talk about soon.
Putting it all together
Nothing helps cement the learning process better than a practical example. Let’s look at someone who has all the cards stacked against them, then figure out how to pull their heinie from the flames. Here folks is Pete “Proteinuria” Paducka.
Pete is a 30 YO male, 175cm tall, 110kg (I can’t tell you hw depressing and embarrassing it is that the US can’t figure out the metric system) and pretty much a mess. He is sedentary, stressed, has terrible sleep and exists on packaged pastry products and beverages with “DEW, Pepper” and similar monikers. Recently Pete had to get a physical and he had: high blood pressure, elevated: blood glucose, BUN, creatinine. Given that his condition was obviously not good it was recommended that his renal function get checked out. Tests indicated Pete was operating on approximately 10% of normal kidney function. Pete was pretty shaken up by his condition…peri-diabetic, facing dialysis ( his doctor wanted to start dialysis IMMEDIATELY) and all at the ripe old age of 30. Fortunately for Pete, his employer was a member at a wacky little gym called NorCal Strength & Conditioning and the employers offered to not only pick up his gym membership for a few months, but would pay Pete on an incentive basis: $5 for every pound lost. This is a small IT company, and I’m sure this situation violated multiple California state “fair employment” laws…but it’s what happened here. Pete went through an initial assessment at NorCal, and it was recommended that he work with Amy Kubal on his nutrition. The course of action involved a low protein (10-15% protein) low carb ( less than 10%) high fat (mainly from coconut products), ketogenic diet. Pete’s doctor was horrified, but we petitioned for one month of “tinkering” to see how things went. Three weeks later Pete’s GFR was 80% of normal instead of the previous 10% and his BUN was within normal ranges. His doctor was interested…but baffled. Pete has subsequently titrated up his protein intake with no ill effects on kidney function.
The Tea Leaves
When you look at the etiology of most kidney diseases the approach we took with Pete addressed every damn variable all at once: autoimmunity, elevated insulin and growth factors, AGE’s…did I miss anything? Interestingly, about a week after Pete got his 80% test results back this article appeared, extolling the virtues of a ketogenic diet for renal failure. As I’m writing this I actually get ANGRY when I realize how much death and suffering occurs because insulin resistant diabetes (and all of it’s complications, like renal failure) is “managed” instead of “cured.” Unfortunately most folks are too addicted to their unhealthy lifeway to change in the way that I’ve descried here…but many will change if given the option, but our government and medical community are still in a metabolic dark ages. Sigh.
I’m sure folks will have questions, please put them in the comments and I can get to these in either a follow-up post or perhaps a podcast. I’d planned on this being substantially longer but I have some events cooking that will take me 100% out of email, phone and similar coms until early July. I’m not sure when I’ll be able to share information about that event with y’all, but I will when I can. Nicki will be Ok’ing the comments while I’m gone, podcasts are in que. Thanks for the continued support and I hope folks find this piece to be helpful.

Great article – thanks Robb!
What would be some typical meals on a 75-80% fat diet, such as the one recommended to Pete?
Would a low-protien, very high fat diet typically be recommended for people whose doctors have told them that they are in a pre-diabetic state, or does that state not always entail kidney disfunction?
B
Great article and thank you for tackling this topic. I’m 23 and just received labwork showing that my kidneys aren’t functioning very well, which is terrifying. Been paleo since 1-1-11, but that apparently hasn’t fixed the damage (yet). I agree with Brent that some sample meals over a day would be HUGELY helpful! Alternatives to nuts would be great, because I want to keep my omega 3 to 6 ratio about even. Again thanks for the much needed post.
Charlie
I know this is a really old comment, but for the people who might be reading this right now, a good sample paleo breakfast might be 1/4 – 1/2 cup grain-free granola (probably mostly nuts and seeds) drizzled with honey or natural maple syrup. A lunch could be a salmon filet, cooked in coconut oil, alongside a greens salad drizzled with olive oil, perhaps 1/4 or 1/2 an avocado. Dinner would be grass-fed beef (cut of choice) with asparagus spears covered in grass-fed butter. Perhaps a sweet potato, if you’re allowed sweet potatoes. This is a paleo dinner. Very few starches are allowed on paleo. Quinoa is actually highly inflammatory and is not indicated for kidney patients.
Hi! I think they were looking for the keto meal options, within the strict parameters given for the kidney disease patient in the post. The lunches and dinner look like OK options, but you would want to add some more fats on the side to make sure the fat percentage is high enough.
Nicely done Robb. Ironically, I had a friend that I recommended read your book and give Paleo a try. She has been following it pretty well as far as I know, but a couple weeks ago she went to her chiropractor. The moment she told her chiro what she was eating and the amount of protein the chiro immediately defaulted to the argument that all that protein is bad for the kidneys and liver. I forwarded this article to her in hopes that she will present it to her chiro. It is seriously difficult to argue with FACTS. This is just another case of someone not looking at the WHOLE picture (e.g. fruits are very nutritious but they still have a shit-ton of fructose and may not be the best option for the bulk of your diet). Thanks again for the opportunity to “stick it to the man.”
Robb,
What would be the standard for GFR and creatinine?
A standard GFR would be @ 120 mls per minute out of which @ 2mls of urine are produced. A standard creatinine clearance would be more difficult as it is dependent on body mass and muscle mass in particular.
Robb — Having been an Atkins advocate for years — KNOWING this way of eating works for me — and having recently read Tim Ferriss’ 4-Hour Body and Gary Taubes’ books (which are especially well researched), I so agree with what you write here. It’s going to take a WHILE for the general public AND health professionals to ‘get” this — but this general way of eating will save lives and create thrilling lives. Thanks!
I’ll eat the twinkie but only with chicken wings so I can get my breakdown of macro-nutrients correct. Oh and I want my 5 fries!
Seriously Robb thank you for clarifing this topic. I can’t tell you how many people tell me how I’m going to have kidney damage and I tell them it’s not true but I don’t have enough bio chem to go into specifically why. This helps!
Thanks,
Ankit
ARTIGO MUITO BOM AMIGO!!!
Keep up the great work!
Cheers from Lisbon
Pedro
Great job on this one! It’s just amazing how the general public and general medical practioner can’t grasp the answers right in front of them .. Treat the problem, not the symptoms PEOPLE:).
Anyway, nice work on the DSKF;) oh I think we all want that, I know i do
Wow, I haven’t read the whole thing yet, I gotta get back to work but this is very impressive breakdown. Fantastic work robb!
What are your thoughts on this potentially new DM drug; a selective sodium-glucose cotransporter-2 inhibitor. It reduces renal glucose reabsorption in an insulin-independent manner. I’m sure a 24 week study is enough time to predict long term safety. If it gets approved, I give it 5 years before it is pulled.
Will Pete’s kidney function improve over time, or will he need to always be on a high fat diet?
Bacon fat? Butter?
Are there AGES is cooked meat?? and if so what percentage and should I be worried about it?
Thanks Robb
This is very helpful – I am considered a Stage 3 CKD with an average GFR over about 5 years of 55 – where might that put me in the recommended percentage of protein/fat/carb consumed? Strangely, although I have basically eliminated sugar, grains, severely limited fruit, etc., my fasting Glucose level just popped up over 100 again. No biggie, but I was severely pissed since I expected it to be much lover–doctors defer to my age (74) although I am extremely fit, low BP, wt., etc. I would also be interested in what kinds of menus would incorporate more good fat and if that would be a good idea for me. I don’t seem to need to worry about gaining weight. Thanks so much, Robb, for making this issue a priority when you have so many demands on your time.
What a fantastic article.
I would love to re post this on my blog http://www.yourfitday.com
Many people on my list have diabetes, and other issues, that can be ‘cured ‘ with diet and exercise. This is a must read for them.
DebbyK!
Good post . I hope that pic of the cute kid is yours, Looks bright and fun.
Hey, Robb,
Thanks for this post! I had microalbuminuria and still have multicystic kidneys (turned out it is not PKD). Low carb lifestyle and vitamin D supplementation cured my proteinuria. Can’t wait to read the next part! It is literally impossible to gain acces to valid info on this topic. Thanks again for writing about this!
Liv did u do animal protein or low carb paleo approach? Also how much vitamin d doseage?
I just had some blood work done and my creatinine levels are high. My doctor says my kidneys are operating at 40% capacity. He is blaming it on creatine supplementation and my protein intake. I am 46, and have been a weightlifter since age 13. I am on a low carb diet. My insulin levels are down, but my cholesterol is 336, and he is alarmed at that, never mind that cholesterol-causes heart disease has been debunked. He told me to stop the creatine and lower my protein intake. At 172 lbs. my daily protein intake is around 130 gms./day. Also, a friend, a nutrionist, says that my creatinine levels WOULD be high due to my training.
However, what my doctors haven’t considered is the fact that, as someone with a life long history of clinical depression, I have been subjected to years of anti-depressants, including six years of the maximum dosage of one particular drug. I have been off anti-depressants for three years. It is my opinion that, if my kidneys are functioning at that level, it is due to damage from the medications.
What are your thoughts on this, and can this damage be corrected?
I am no expert, but I might wonder if your protein intake is too low, and therefore eating your own muscle mass creating excess creatinin excretion. If you are training hard you might need more, and hopefully your calories are at a good level. Good luck and God bless.
My suggestion is that you get off anti-depressants as they do more harm than good. The whole narrative of a chemical imbalance in the brain is bunk. Check out what Dr. Peter Breggin has to say on psychotropic drugs. He has some 20 books and you can see his videos on Youtube. Here is a link fro one of them. I was on lithium and others for 14 years and I was fortunate to be able to get off the, Psychiatrists had convinced me that if I stopped taking them I would get a breakdown. In 16 years no such breakdown has happened. Good luck.
great post, very informative thanks
Roberto,
Reading that was a test of mental fortitude, but necessary. Next step, perusing iTunes U for some open biochem lectures. Any suggestions?
Robb,
Thanks for the enlightening article. It will serve as good ammunition for the misinformed masses.
The one issue that caught my attention was the nighttime urination (you briefly mentioned this topic in your book, too). I wake up to go to the bathroom almost every night and I assume this nuisance is due to elevated cortisol levels rather than hyperinsulinism; I eat moderate-to-low carbs, am a lean athlete, and have found that meditation improves the “condition” a good deal (whether or not this is due to placebo I don’t know). I also think I have pretty low sex drive for a 19 y/o if that means anything (I’m guessing that the cortisol, poor sleep, and lagging hormones are bound together in a vicious cycle).
I’m guessing that I could get rid of most of my issues if I cut back my bacon addiction and was more consistent and “intense” with my meditation, although whatever wisdom you can provide would be greatly appreciated.
Thanks a ton,
Robert
Hi Rob,
Donating a kidney to my sister tomorrow morning (Stanford).
She has IgA nephropathy (Berger’s disease).
My mom has Celiac. I gave up wheat two years ago and have experienced an incredible turn around in health (240 lbs BW to 180; IBS/constipation: gone; chronic stomach ache: gone).
My sister tested (once) negative for Celiac. The docs and nutritionists (arguably some of the top guys in Nephrology in the world) don’t give a rat’s ass about the fact that my sister’s brother and mother are completely wheat intolerant. They couldn’t care less that Celiac is an auto immune disease as is Berger’s, and they don’t think she should give up wheat.
My sis says, “My stomach doesn’t hurt like yours did. I tested negative for Celiac, unlike mom. The STANFORD nutritionists and DOCTORS don’t think wheat is a problem.”
Well f*ck man she’s gambling with my kidney from my point of view. Or am I just trippen out Rob, nerves and all, night before?
Thanks. You rock.
PS remember that Ray Mentzer died two days after Mike? He died of complications due to Berger’s. ANywho…
hi robb- what about people who can’t digest nuts? some of the recipes have nuts in them – thanks
Hey Robb, I donated a kidney to my brother 6 months ago my new kidney function is 72%. Are the any changes for the person with the solo kidney? Are creatine supplements out of the question?
Fantastic article. I will reread this a few times with the links. I am obviously metabolically deranged. I have gout and some high BUN and creatinine. YOur article got me thinking about something. I cramp a lot. I have pretty much gotten used to it. I wonder if it is because of increased aldosterone. What do you think?
I’d rather not discover that I’m eating too many green vegetables by getting kidney stones (and besides, how would you tell? Green stones?). How can one be sure you’re eating enough, but not too much, spinach, romaine, greens, etc.?
Hey Robb,
I’m 22 and recently got a blood chem done. My BUN is high at 29, creatinine was normal at 1.15. Protein was 7.3G/dL. I eat high protein paleo and I’m fit and healthy afaik. Im trying to figure out why kidney function isnt ideal. Maybe a high (80) vitamin d level isn’t helping my kidneys? Any insight into this high BUN would be truly appreciated. Thanks for your time.
Read the Kidney Confusion – Intro yesterday & left a comment. Now found this article; thanks for the further clarifications! Hope it’s not too late for me!
I guess that makes sense.
This is not the right website obviously for dog health… but I think that most of the information applicable to humans with the paleo diet is similar to dogs except the meat should be raw when fed to dogs… Anyways I’m curious if the aforementioned caloric proportions would be applicable to dogs with renal failure (10-15% protein, 10% carbohydrate, 75-80% fat) or if humans are more capable of fat adaptability than dogs are. I don’t want to feed him too much protein and induce kidney stones, and I don’t want to feed too much carbohydrate and maintain the metabolic derangement. I know you are not a dog expert, but maybe you know about gatos. And maybe the gato kidney function is similar to the perro kidney function.
Seems good to me. find a vet who gets evolutionary biology.
Cats & dogs have very different digestive needs. Dogs are omnivores, and cats are obligate carnivores, so important not to generalize between cats and either dogs or humans! Best info on the cat version of a Paleo diet: catinfo.org. Perhaps Dr. Lisa, who runs that site, can point you to proper diet information on dogs.
Although it’s too late for the OP, for anyone else reading this: for heaven’s sake, do NOT assume what might be good for you is good for your dog. A diet of 75-80% fat is not appropriate for a dog. You can easily induce pancreatitis in some dogs with much less fat than this. If you have a dog with renal failure, google for Fuzzerfood (although this is primarily a diet for kidney stones). There is also a Yahoo group, K9Kidney for dogs with renal issues. They can provide real help, especially regarding diet.
Hi Robb,
Last year in my annual med tests exam my doc found blood in my urine. He re-did the test with the same result. Sent me to get an MRI of my kidneys, they were fine.
This year he again found blood in my urine. My blood test shows elevated potassium (5.7 mmol/L), plus slightly high ALT, and slightly low WBC, RBC and lymphocytes.
Doc’s secretary said everything was fine when I called to check on my results but according to this post and other sources I’ve found online, high potassium in blood is closely linked to kidney issues. Is this something I should be worrying about or is this slight above-the-range levels not serious?
Thanks in advance!
I went to hospital with gout symptoms in june:
Blood uric acid – 9.4
Blood urea nitrogen 28.3
Creatinine 1.26 (at 5’11 75kgs reasonably athletic but not huge muscle)
Doctor wanted to give me meds to lower uric acid but that seems to me to be treating the symptom not the cause (kidney disfunction) so I declined.
According to this I should try a ketogenic diet – low protein (10-15% protein) low carb ( less than 10%) high fat (mainly from coconuts).
Does that look about right? Biochemistry is hardly my field so I’d be very grateful for a little reassurance as I start this new diet (already been paleo for about 9 months). Thanks for anything anyone can offer!
Hi I have been trying to find out some information regarding living a paleo lifestyle for a person who has had a kidney transplant. A friend of mine has been following it now for a few days but understandably has major concern about what the high protien levels are doing to his one kidney. Doctors don’t seem to agree with paleo fullstop so I can’t see him getting unbiased advice there. Any information anybody has would be greatly appreciated. Thank you, Noreen.
Noreen, Paleo doesn’t need to be a ‘high protein’ diet. It can be modified to fit the needs of your friend. I would highly encourage him/her to stick with it and if I can help let me know! http://robbwolf.com/about/team/amy-kubal/
I am very confused. I had a 24 hour urine test. My protein was within normal limits and my Creatinin was also in the normal range. But the protein/creatinin ratio was high. It was 180. How could this happen?
Thanks for posting this Robb! It is very encouraging. I’m a 34 yr old female, i’ve been doing crossfit, dabbling with Paleo, and of course, listening to your podcasts for about a year now. I recently became ill with a viral syndrome and shocked to find my kidneys go from 40% to 20% normal kidney function within the last 3 weeks. You can imagine my shock as didn’t even know I had a kidney problem to begin with….and I do not have diabetes, high blood pressure, or hypertension. Needless to say, I am very confused as we are not yet sure what the cause is for the failure. I began to question many things, including this lifestyle, but because of this post, I feel more confident in the path I’m taking as I now feel like I may have the the upper hand and have a plan of action better suited for my situation. I’ll be continuing crossfit and Paleo and following the recommendations to watch the protein (.8/kg), potassium and phosphates and hope to have a story similar to Pete “proteinuria” Paducka’s very soon! Thanks again!
Wow, while this is undeniably and impressively thorough, I’m ashamed to say I can’t follow hardly any of it. I’ve tried a couple times.
I’m a male under 30 years old, 5’10”, clean medical history, and 165lbs. Relatively lean. Recently had 2 excruciating kidney attacks within 2 weeks of each other. The first lasted 4 hours while the second lasted about 48 hours. Brutal. I’ve been on paleo for 2 months, with high fat, pretty high protein, and low carbs. It seems so compelling that ingesting so much more fat and protein has caused this condition in me…but as you say, I must have had a damaged kidney to begin with somehow. I have no idea what was wrong with my kidney to begin with, and now I have no idea what to eat to remedy the situation. Of course my doctor says cut back on beef and chicken. No idea if that’s good advice. I wish this article allowed more practical applications to move forward in some kind of sane manner, but I get that you have to lay out the science. No idea where to go from here though. Low carb and low protein maybe? How in the world is that possible?
I’d agree with Robb that you likely had something in the works before the “attacks.” Important to figure out what kind of attacks. Were you passing stones? Stones probably don’t form in 2 months; they’re gradual, and for some reason they just moved. It could be they moved because of getting *smaller*. There’s really interesting data available on stones and crystals from a lab called LithoLink – your doctor can order an analysis. You could then find out what you’re predisposed to, and even repeat the test in a year and see if a Paleo diet is making you better.
Hello! This was very thorough text, liked it! I have a question to which I haven’t gotten any satisfying answer from anywhere:
I am 27years old female, 171cm and 65kg. I have lost about 25kg’s mainly by eating less and moving more. Now I have a desire to lose the rest of the fat in unwanted places on my body (such as stomach, arms, thighs..). I was diagnosed with very early stage and good-grade IgA -nephropathy in 2010 so that my urine-&bloodlevels that are important to monitore in this illness have been just above those levels of not having healthy kidneys. This diagnose motivated me to lose weight, to move more and to get as fat-free and trained body as possible (in the limit of good-looking ;). My blood pressure has been excellent these years (usually about 110/70, max 120/75) and I’m in good shape except I hate the fat that covers my abs and the flap-flaps in my arms etc, typical women problems 😀
So I am determined to get rid of those once and for all. This is why I have been on a diet and exercise -plan which I bought from a company called FitFarm. They have this program for example for people who wants to lose “below 10kg”. It is 6 weeks long and I have been on it about 5 weeks now. Because this is ending, I think I have to come to a conclusion about how I proceed.
The training part contains of 4 extra fat burning workouts per week, which are done with low weights and bodyweight and take about 1h-1,5h. They are really intense (so called giant sets) and the heart rate is up all the time and you are really sweaty. In addition to this you have to go and walk 4 times 45-60min per week. I have done all these and in addition walked my dog about 7times/week. So my weekly training hours meet 15h.
The program contains a diet of which calories have been going down since the beginning. First they were about 1800kcal/day, now about 1300kcal (training days are 1500kcal). Now to the problem finally: Protein intake has been very high! Now it is about 156g/non-training day, 187g/training day. The discussion about the “right amount of protein because of kidneys” is very variable.
I have no intention of losing my kidneys. I think I haven’t done much harm to them because of this diet which has been on only for 5 weeks now. But somehow I think that this really isn’t healthy for me to eat that much protein in the future? Maybe even stop already.. I have my yearly urin-&blood tests next week. It is really interesting to see if this have had effects on me, I hope not.
So basically I am asking if there is a good protein intake amount for me which prevents my body of using my muscles during a diet and instead it uses the fat I have? Thank you very much if you have had time to read this. Those protein intake amounts which I just counted are very shocking for me.. I didn’t realize how much of protein I have been eating. I hate that I don’t have healthy kidneys 🙁
Something more about the diet, so you are more aware of this thing if you answer:
Every day I eat&drink (only relevants concerning my problem):
– 3-4 liters of water (usually 3-3,5l)
– 5 g added salt (in all 6,4g)
– 200 g low fat meat/chicken/fish (half during lunch, rest in dinner)
– 500 g quark (non-fat) (half is in breakfast, half in snack)
– 270 g cottage cheese (non-fat) (a bit in big meals and 200g before bed)
– also berries and green vegetables 600g and a bit pasta/rice and fats from good resources (like olive oil and omega3)
I hope you have time to think my situation. I really haven’t found any help from anywhere. Nobody seems to understand that I would like to have muscles and a trained body and look good in bikinis, and not to be “skinny fat”. What would you recommend as my protein intake from now on? Thank you!
Robb, thank you for the article. My wonderful boss turned me on to you this morning after I found out that my 15-yr-old son will be scheduled for a kidney biopsy in a month. He has had protein in his urine since December, for which he is being treated with prednisone, but he is not getting better. Being Asian, he loves rice, so removing that from his diet will be difficult. What should I do about protein (meat) intake? He is constantly hungry (and fatigued). Can I still give him his favorite meats (chicken, beef, pork)? He is on a low sodium diet to reduce his fluid retention. He has gained 10 lbs of fluid weight in the last month (could also be due to his prednisone). He is 5′ 5 1/2″ and weighed 114 lbs prior to all of his kidney issues. Thanks, Robb! As you can imagine, as a mom, this is making me stressed as he is scared about what is wrong with him.
Hi Robb,
Great article. I am 40 years old in stage 4 chronic kidney disease…. i am about to start the ketocentric diet but the one concern that i have is that i have high amounts of potassium in my blood (6.3 at the moment) and so much of the fats have high potassium in them…ex. avocados,coconut oils etc… do you have any thoughts about my concerns? would it be wise to wait to start the ketocentric diet?
Jake!
Not sure how coconut oil has much potassium, but clearly you need to monitor that. I’d reach out to Dr. Phil Blair and see if he is willing to work with you. He is quite knowledgable in this area.
Keep me posted.
Jake, how has your potassium level been? I am working with a patient who has a similar situation to yours–high blood potassium and her total protein is low (below optimal) in her blood. We’ve started on some digestive support to help her produce more stomach acid (she is on Nexium, which is just blocking her from properly digesting her food). Her history is very extensive so there are a lot of factors, but I am wondering if the Paleo diet helped you? My patient is going to working on getting the wheat out of her diet and artificial sweeteners (she consumes A LOT of these daily). One step at a time, but I am hopeful. I would love to hear your update–thanks in advance!
Hi Robb, I’ve been experimenting with Paleo for about four months, have lost 10lbs and stayed there. I am not metrically inclined, sorry, I’m 5’10” and 170lbs, mother of three young children and trying to get a little active. My father had a kidney stone and my grandmother is having kidney problems at age 90. I have have been feeling better than ever on Paleo diet but noticed I am a bit colder than usual, have noticed line indentations around my ankles from socks that are unusual, as well as more frequent urination. :(. Should I be worried? Also, if a person eats a low protein 10-15% low carb 10% ketogenic diet what does the other 75-80% of the diet consist of?
Well, if it’s ketogenic it’s relatively high fat. Have you had renal function checked at any point?
I have never had my renal function checked because it was never a concern until family members mentioned started having problems. It might be hereditary eh? I will get the doctors opinion. I thought maybe I felt colder because I lost the 10lbs.
My added question is more a confusion than anything. My husband and I eat almost strictly paleo with several exceptions, butter, coffee, small amount of yogurt, some rice, and popcorn. I am uncertain about your article example of Petes diet above and what the low carbs at 10% are. I thought the carbs in Paleo came from veggies and protein from meat and that was that.
Thank you!
Robb,
I have a question is about uric acid kidney stones.
“7-If you get kidney stones that are from urate salts, you are likely NOT following a low-ish carb paleo diet, you likely have insulin resistance and your liver is not processing uric acid.”
Can you explain more about how the liver doesn’t process uric acid properly? My understanding is that the liver’s function is to produce uric acid. The kidneys then remove this uric acid via urine. When the kidneys don’t function properly BUN rises and Gout can result. In what way does the liver “process” uric acid? And how are uric acid based kidney stones formed as a result of improper liver function?
Thanks
John! Let me do a follow-up on this where we look at the effects of gluten on the liver, inflammation, insulin resistance and how that all affects this story. I think that’;d be valuable for a lot of folks
Metric Conversion: (Given the author’s stubborn nature)
243 pounds, 5′ 9″
Robb,
I have been following a Paleo diet and CrossFit for about 3 years now. I have been pleased with the body composition changes, but have had injuries. I am not 100% Paleo! but try to limit the bad food I eat. In the last 2-3 months I started to incorporate Progenex Muscle and Recovery supplements on the days I did CrossFit. With two trips to the ER in the last 3 months for a shoulder injury/pain thinking I was having a heart attack and severe stomach pain, the ER Dr noted that my Kidney Filtration Rate has decreases and has referred me to the Neprhology Clinic. I know I leaned more towards protein based diet in the attempt to bulk up. Now I believe maybe the supplements and protein heavy diet has damaged my kidney functions? I am interested in the Ketogenic Diet to see if I can reverse the effects? In the article you mentioned a fat based diet on coconut? Do you have a link to a sample meal plan that I could try for a month to see if I can have the same results.
I am 51 years old, active. 175lbs, 5’10”
Last reading Creatine about 1.58 and EGFR about 55?
Any information would be very appreciated.
Thank you,
Richard
Richard-
I do not have an off the shelf meal plan…not a bad idea for us to put one together. This is some of my concern re protein powders…they hit the system so quickly it’s really not comparable to solid food. Keep me psoted.
People who want ideas on how to eat high fat low carb would benefit by looking at this web site: https://www.reddit.com/r/keto/ also https://www.reddit.com/r/ketorecipes
So just a question if anyone has some tips. Age 35 type 1 diabetic started ketogenic paleo about two weeks ago. Should renal function increase with this type of lifestyle? Am I just delaying unavoidable dialysis? Really want to tell my doctors where to go!
Hi there,
I am a 30 year old male from the UK. I was diagnosed with IgA nephropathy almost 18 months ago (by chance too, I work as a Health Surveillance Technician and a patient didn’t turn up for a medical one day so I tested my own urine instead!). I found ++ protein and ++++ blood in the urine. Contacted my GP and was escalated to Renal Specialist. More and more tests were then conformed by a biopsy. About 15 months ago I was advised to go on a trial….125mg of Prednisolone every other day for 6 months. Most people will never go over 20-25mg of Pred per dose so I was kinda worried by the levels they wanted to put me on. I was even more horrified when I read the list of side-effects! Being on something so aggressively catabolic meant that I had to take a whole other bunch of tablets for stomach, muscle, bone as well as being advised to take glucosamine, cod liver oil and a few others. After some research and some long chats with the Specialist I decided to give the trial a go (mainly due to the fear factor of needing dialysis in the next 5-10 years).
I’ve had 2 blood and urine tests since finishing the trial (by the way, the only side effect was some facial bloating and mild acne on my back). I controlled diet by almost eliminating salt, reducing red meat to one meal a week, cutting trans fatty snacks, upping the fruit and veg and lots and lots of water. The results have restricted the level of kidney damage. I was never given a grade or a level to my knowledge. The tests took place when i fisrt come off the Pred and 6 months after. The results have been good so far but with there only being two sets of results there is little clarification on the desired ‘Legacy Effect’ they were looking to achieve.
My point for contacting was to ask a simple enough question. With my history and potentially underlying condition am I able to take on diet-based protein at will? I am getting married in May and I’d like to lose a little bit more weight (currently 80kg at 176cm, considered overweight on the useless BMI chart). I also want to get ‘cut’ in respect of muscle definition. Secret: I have a little muffin top that needs to go! lol
My gym friend has recommended some fat burners and an all-in-one whey shake but I have reservations about the content and how it may take its toll on my ‘status’. I know lots of people will say ‘stay natural’ and ‘there’s nothing wrong with your stature’. Although these things are true I could still do with the pointers, even if for education purposes more than anything.
I have heard various reviews on the ketogenic diet and Paleo but not entirely sure what they entail or how to impose them but if anyone has any thoughts or recommendations from a nutritional point of view I would be very grateful.
All the best form the UK,
Simon M
I’ve seen others ask this with no response. Hopefully, I’ll get one.
I am a 47 yo female and I donated my left kidney to someone 6 months ago. I have started on paleo and will probably switch to autoimmune protocol soon. My creatinine and BUN are higher than they were in Dec. (pre-paleo). Should I limit my protein intake or give my remaining kidney time to increase its function?
I would highly recommend consulting with Amy Kubal (one of the great RD’s on our team) for this issue. http://robbwolf.com/about/team/amy-kubal/.
My mom was diagnosed with renal failure. Her kidneys are at 10% working capacity the doctor recomended dialysis but she strongle refused then he recommended the keto diet. I will like to know the percentage of keto diet fat, protein and carb. Please answer. . Thank u
Hi Robb. Aussie Male, 32, 6’4′ 180 lbs. Training for triathlons and eating mostly around 200g a day of carbs (fruit, oats, vegies) with plenty of canned tuna and other meat. I have recently switched to a Mediterranean type diet with more organic butter and cheeses. I have tried a few processed meats (salami, ham) lately which I havent eaten for a long time. Have noticed foaming in the toilet when I pee, which I have read is a symptom of protein in the urine. Do you suggest trying the above mentioned ketogenic diet (10:10:80) and see if the foaming reduces? (I have tried very low carb diets before)
Cheers mate.
Hi Robb,
I lost my
Left kidney to kidney disease and reoccurring pyelonephritis in 2011 at the age of 26. I was diagnosed with Hashimotos in 2013. I have since started a Paleo diet and just finished 30days of AIP where I have now got the first Kidney infection I have ever had since my nephrectomy. Do you think this may be from the high amount of Protein as it’s the only thing that has changed. I have eaten Organic for 5yrs so baffled and as you can imagine quite scarred with this current infection. I hope to hear from you soon.
I have kidney problems. What kind of diatribe should I be on. You see I was born.with one bad kidney and did not know it it’ll my create levels jump 2.7. I resets it to 1.6 now back up to 2.0. Now how do I get it back down to to below 1.2.
Hi, I have had my transplanted kidney for 10 years this year. I have poly cystic kidney disease and hypertension which caused me to go into end stage renal disease at the age of 20. All of my levels are doing excellent ( I lied my triglycerides were a little elevated) and was wondering if I should try the keto diet? I am going to ask my Nephrologist, however I do fear that he will simply object, however I have been struggling with weight loss for awhile and feel it is more damaging to be overweight then to try the keto diet. What would you suggest?
Patti-
I think there are compelling reasons to consider this option. Your doc is unlikely to know that KD’s are low protein and well documented in cases like this. Good luck and keep me posted.
I have been attempting a ketogenic approach to weight loss. First 2 weeks, I had great success with 50g net carbs (at least 20 fiber to keep GI doc happy) and 90-120 protein the remainder being fat. I was also keeping it under 2000 calories per day. I’m a 5’10 300lb woman so this is pretty good deficit. The weight loss has stopped at 50g and I’m thinking of going lower. We traveled for Easter and I did not keep the 50g going but now can’t seem to get back into Ketosis. I have kidney damage from infancy and lost about 40% use of my kidneys at that time. I have had trouble in pregnancy because of this and always my albumin levels set docs in concern unless they know what happened to me as a baby. Now I’m worried about dropping my carbs lower, even for a short time, to get ketosis going. What are your thoughts? If I drop net carbs and protein does that help keep me safe? TY in advance!
In general dropping carbs and protein WILL enhance ketone production.
Dear Robb
In India I have seen patients undergoing dialysis recovering by doing Kapalbhatti, a pranayam (breathing pattern). Baba Ramdev and patanjali trust have case studies but i have seen ordinary persons become better. Look your art impressed me a lot. I suffered a stone 30 years back and almost lost my life. I have seen alternates like acupuncture work for some. But kapalbatti is like magic. What the heck. patients have nothing to lose except their disease.
I am diabetic but blood glucose is under control which is due to exercise. I jog about 10km every other day completing it with exercise of about 45mins. It includes about 60 to 90 push-up, 200 sits up, two sets of planks (left, right and front), 10 chin ups and 10 pull ups. On days when I am not jogging I would do the exercise only. On every wednesday night, I play badminton strenously for about two hours. Laterkt before my checkup I ride on by bike for a total of 70kilometers. My creatinine shoot up to 148. On top of it I am 90% vegan which cause my Vit B12 and blood cell count to be low.
Given these factors, do you think that I have CKD?
Appreciate if you could comments. Thanks
The only thing I’m pretty sure of is the creatinine is likely due to the exercise volume…but you should def have followup work to establish that.
http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1523335/
paleo while kidney impaired study
Nice find!
i am a female, 65 years old. I have type 2 diabetes, hypertension,. I was diagnosised with stage 3 kidney disease on 5-4-15 with creatinine 1.20 and GFR of 46. As of 9-17-15 my creatinine went to 1.50 and GFR down to 36. I am 5’5″, did weigh 241 now down to 213 and continuing on a low card diet.. Hopefully will obtain a weight around 160-170. Just was taken off Metformin yesterday. What do you recommend for me to do. Do you think I have any chance of lowering my creatinine and raising my GFR?
My father died from kidney disease He had been an athlete in his youth but was overweight when he began to have heart , blood pressure and then kidney problems. I started to look for alternates to his unsuccessful
health -through – drugs strategy when I turned 55 and my peers were becoming obese. I read Dr. Cordain’s Paleo Diet for Athletes and your book The Paleo Solution and started on a casual Paleo diet in 2009. In neither of these books did I ever see a diet recommendation that was high protein or low carbohydrate. The Wahl Protocol is pretty much the same. Lowering the amount of denatured food from the diet is not the same as lowering carbs tho it can be. Including meat in the diet is not the same as a high protein diet. Eating 9 cups of veggies per day as per the Wahl diet recommends will certainly provide carbs. Meat in the 20/80 ratio as per the Paleo diet can’t ever be called high. I’m at around 9% body fat now eating all the ( blood vessel clogging) fat I can add to the vegetable and meat diet. My latest cholesterol test was off the chart low and my blood pressure is normal. I don’t believe in the genetics thing anymore. You are what you eat.
I am 65 and just diagnosed with stage 3 CKD. Creatinine 1.50, GFR 36. My diabetes is under control as is my hypertension. My doctor just took me off Metformin which I was on for 7 years. I never before drank very much water which I am now trying to drink 60 to 70 OZS a day. Have lost 25 lbs and have another 50 to go. What do you recommend for me todo? Can your creatinine level ever come down and your GFR go up? I have been eating very low protein, with mostly chicken over the last 7 weeks.
There are specific ketogenic type diets that are supposed to work well with CKD. I recommend consulting with Amy Kubal (RD on our team), as she’s worked with a number of kidney patients https://paleosolution.frontdeskhq.com/offerings
My father is type 2 diabetic, hypertense, has renal failure and he is on peritoneal dialysis, is it ok to do a keto diet doing dialysis???
Thank you.
My father is type 2 diabetic, hipertense, has renal failure and is on dialysis since last year, he has had days ago a subdural hematoma surgery, it is safe for him follow a keto diet???
Hi,
Thank you for the simple breakdown in your article. I am a 33 y/o female with rapidly declining kidney function. I have been diagnosed with iga nephropathy. I am otherwise pretty healthy; healthy weight, normal blood pressure, no diabetes. I eat all organic foods. I was excited to hear your ideas about diet, etc, but then as I dug a little deeper I found that your example, the linked article, etc where people experience a turn around was those that also ate poorly, had diabetes, etc. I am wondering what ideas you have for someone that doesn’t have all of the other issues that usually accompany kidney disease?? Please reply.
I’m not diabetic or have high blood pressure, I do have high protein in my urine and high microalbumina. Should I cut down on proteins? My doctor doesn’t think there’s a problem. Should I be concerned about this? I am 65 yrs old and generally fit
I am 68 year old white woman. I had a subtotal thyroidectomy a long while ago. I have suffered from high and low thyroid function since then. I have high blood pressure and Hashimotos thyroid. My thyroid is very hard to control. I am borderline diabetic also. My question is how much does the thyroid affect CKD and why does no one talk about it? I need some direction here.
Thanks
apollohospital
Robb,
Thanks for the informational and thought-provoking article. At age 27 I was diagnosed with renal cell carcinoma. I had my right kidney removed and have been living well since with only minor health complications. Now at 35 my creatinine levels are rising leaving me at Stage II renal failure. I lift weights, run and figure skate maintaining an active lifestyle and ideal body weight. Over the last year or so I’ve been experiencing intense GI complications. I’m considering a Keto lifestyle in an attempt to rid the discomfort I get with eating dairy and wheat-although all tests indicate no allergy to these foods. Before I go all in, I’ve been warned by my doctors (GI, Nephrologist and Urologist included) to keep my Protein intake low. Your article makes me think twice about their advice. Thoughts?
Thank you!
AJ
In the case of having pre-existing kidney disease, and only having one kidney, then keeping protein intake lower may be in order. If you would like some specific help, I highly recommend consulting with Amy Kubal. She’s one of the great Registered Dietitians on our team and would be able to help you optimize your diet and nutrition for your situation. You can take a look at her page and rates here https://paleosolution.frontdeskhq.com/offerings.
It will take a while to digest this article, so to speak! I have been eating keto since May, lost 45 lbs, down from 225 to 180 and inflammation seems a thing of the past. But worried about kidneys as some advise against keto for those with a history of kidney illness. I had episodes of nephritis as a preteen and then again at 30. (52yo now.). But I keep thinking if the amount of protein in my keto diet (~25%) is no more than what it was previously how could I be harming my kidneys? Doc agreed to run some blood tests, typical ones for kidneys but your article introduces some metrics I had never heard of.
So for someone facing potential dialysis, would an AIP diet be a prudent thing to do?
Possibly, if the kidney issue is autoimmune related. If it’s not autoimmune related, then it could be the AIP might be unnecessary, but a low protein ketogenic diet could be therapeutic. I’d recommend consulting with someone like Amy Kubal on an issue like this.
Thanks for the article Robb. Started Low-carb, Keto and PAlex Diet a week ago. Was on Atkins in the late 70’s. I was diagnosed with PKD stage 4 kidney disease 2 1/2 years ago. Genic…2 cousins diagnosed also. Haven’t been to a doctor in about 14 mos. Moved and haven’t picked a doctor yet. I’m hoping this will help me. Anyone with PKD you’ve come across that has been helped? My urine used to be strong smelling, now no odor…smells like water. I also got a new filtering system that virtually filters out everything including floride. Also went organic veggies and grass fed meat.
I’m pretty sure Amy Kubal has some experience with some patients with PKD. If you would like some specific help, I would recommend consulting with her. You can take a look at her page and rates here https://paleosolution.frontdeskhq.com/offerings.
Thank you so much for this article. It has cleared up a lot of confusion and concern for me. I am a female who lifts weights and has decent muscle mass, especially for a female. My creatinine is 1.14, and my GFR is 58. All of my other test results such as BUN and urine are completely normal. However, I am required to get a physical for work as a law enforcement officer. I feel my levels do not come out as “normal”. I have to see a specialist at my own expense and get e doctor to sign a statement that I am fit for duty. Is there anything I can do in the days before my physical exam to get my creatinine levels down and GFR up? Would it work to not lift a few days before the exam? Thank you.
The description of Paul is scary because that was me 4 years ago. I was 3 weeks from turning 31 when I went to the hospital with breathing problems and lack of energy. Instead of changing my diet, I did what my doctors told me to do and went on dialysis. If I knew there was another way I would have taken it without hesitation. I now have a transplant (9 months ago) and doing good. Transplants have their own challenges but I am hoping the worst is behind me. I still need to make some lifestyle changes but I recently joined a gym and I have decided to try the Paleo diet. I am still figuring this out but after reading this you have given me some pretty clear ideas on what I need to do. Thanks for breaking this down in a way I can understand it and use it.
I am in my late 70s and my kidneys are 50% functioning. I want to go Paleo to lose some weight; is this dangerous due to amount of protein? Hope to hear from you soon. Thanks.
Hi Rob,
I am from India and stumbled on this article as my mother (Diabetic/Uric Acid problem/Cholestrol) – was diagnosed with 2.9 creatinine, 68 Urea, and 4.61 Albumin in her Kidney Function Test.
I would like to know if Ghee (clarified butter) can be a substitute to coconut oil, if incorporated in her diet?
Any thoughts on this study which shows tumor growth INCREASED in ketosis?
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4759602/
There are some cancers which do appear to become more aggressive with either ketosis OR fasting. What is unclear is if the protective effects of a KD+conventional therapies will end up being a net win in a situation like this. Other cancer, like glioblastomas, appear to respond quite favorably to a KD. At best a KD will end up being a tool in the tool box, not a cure-all.
“The HFKD was prepared by Morawski (Kcynia, Poland) from lard, butter, corn oil, casein, wheat bran, a mineral mix, a vitamin mix and dextrose. The nutritional profile of the diet was: fat 79%, protein 9.5%, carbohydrates 0.8%, fiber 5%, vitamins and minerals 5.7%”
This I know something about. As an NF1 patient I got rid of my tumors with a totally meat and animal fat diet. I don’t consider 9.5% carbohydrate diet adequate for fat adaptation. Curing or stabilizing cancer relies on depriving it of sugar. Otto Warburg proved this in 1928.
9.5% glucose would make tumors thrive.
I am at Stage 4 CKD and my doctor informs me that my kidneys are storing dangerous levels of potassium. Will a keto diet naturally reduce the high levels of potassium in my kidneys? Shall I eat 80% or more of coconut oil?
Hi Robb,
For the past year my eGFR levels have consistently decreased (between 45-55). All my other readings and kidney ultrasound were normal. I have Hashimotos disease, about 30 lbs overweight, yet I work out daily like a maniac and also do a Spartan race about every 8 weeks. I just started the Ketogenic diet a week ago and have lost 5 lbs and regained a lot of energy. I am planning to have my labs done in a few months so it will be interesting to see the results!
Hi Robb,
I have arteritis and NF1. The arteritis left me with a permanent essential tremor. I have been on a meat and animal fat diet for about a year. It’s reduced my arteritis and NF1 symptoms to obscurity. A few weeks ago I had a full blood workup for my tremor. My BUN came back 28, one point above range. My kidneys seem to function fine, however.
1. Is BUN damaging me physically in any way?
2. Am I doing something wrong, and need to fix it?
Very interesting article. I had an argument with my nephrologist just today after my kidney reading returned 35% today instead of the normal 40% I have been at for the past 2 years after they put me on blood pressure meds to bring me down from 210 to 130. I am 45 and only weigh 70kgs so weight is not an issue for me. I have a kidney nephritis. So my question is. I have been on Keto for 4 weeks now and the doc lost it when i told him saying I am eating too much protein and cutting 1 food group in favour of another is wrong. I understand the protein thing and will now go about dropping it from 100g per day to his recommended 60g per day. And then upping my fats to cover the difference. But then how do I go about working out with weights in my plan to get up to 75kgs with 10-12% body fat?
I have had proteinuria for 23 years and my creatinine and gfr are in normal ranges still. I switched to vegan diet years ago and believe that is what’s keeping my kidneys from failing. I do eat a good amount of plant protein and don’t consume any processed sugars or junk food and also eat low sodium. My nephrologist is amazed my kidneys haven’t failed. I am obese though and have some blood pressure problems so I’m trying to lose weight and it’s not easy. Any advice?
You might want to give a lower protein keto diet a try?
Hi,
In case of Children with Nephrotic Syndrome,can egg,meat and fish be included in diet?
Hi I just read this today after a lot of research trying to figure out how to improve my kidneys. Here’s a very good study showing remarkable improvement with grape seed extract.
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5083963/
Also theres a lot of studies and evidence nicatonic acid/b3 can help with ckd as well as the known lowering ldl and raising hdl effects.
Theres another very well document bile salt know as TUDCA tauroursodeoxycholic acid the works wonders on liver functions as well as a many other aspects involving the endothelial reticulum.
Please everyone read and research these things!!!
I have none of the usual “markers” for chronic renal disease, although I am overweight (but no hypertension, not diabetic, never touch alcohol, don’t smoke) and am over 60, yet I recently was in the ER for an animal bite infection and the bloodwork came back with a GFR <60 & I was informed I was in danger of renal failure. WHAT??!! I had been on the Keto Diet already for 2 weeks at that time. How long does it take to bring that number up?
Hi I’m 52 yrs old i found out I had glomerulonephritis when I was around 20 years at which my function was 75% I am now stage 3 and my function has been up and down over the last few years atm they are on 43% I have been on the ketogenic woe for 7 weeks I go to the gym 3-5 days a week doing cardio and weights…I’m confused about the electrolytes because apparently kidneys control this,my last blood test showed my sodium was in normal range but on the lower end of the scale and my potassium was also in normal range but on the higher end of the scale.. as for magnesium I have no idea but I am taking a magnesium suppliment… and for people with kidney issues are meant to watch their sodium intake ( so hence very confused) I was having around 80g of protein but I have cut back to 50g because of my kidneys but I’m concerned about doing weights because usually you need more protein when weight training ( again confused) also I have high cholesterol which iv had for years apparently because my body makes too much .. I’m not on meds anymore because I know cholesterol doesn’t cause heart disease and I was once told that your body wont make more than you need! Do I stay on keto?? Do I continue weight training and do I keep my protein low and should I be taking more salt 🙁 please help me I am really lost with all this!!
Robb you have likely forgotten about this article you wrote in 2011 but it is still proving valuable. I smashed up my kidney in a car crash so needed to know more about the test numbers i was seeing from the Drs. Thank you for authoring an article that is clear, concise, and recognises the inherent uncertainty of medical science. Note that whenever i am Googling for info on the body i preface the search with ‘paleo’ so as i narrow the results to someone able to critically assess information rather than regurgitate text book answers.