
I’m appalled constantly at the misinformation we nutrition experts are telling folks with diabetes. It’s all over the place. The “everything in moderation” mantra, and how we need to eat less meat, less fat, and more whole grains, is a pervasive theme drilled into young dietitians, and spread to the public through our dietary guidelines. This information is making people sick.
Last week, the following ad popped up in my Facebook newsfeed several times for “10 Foods That Are Great For Diabetics“. (This click bait article is also making the rounds on several other sites.) Here are the foods: dates, berries, garlic, flax seeds, apples, broccoli, oats, melons, kale and barley. Now, I don’t think that kale is BAD, but this list is like telling alcoholics to drink a little more orange juice or sprinkle some chia seeds into their martini and omitting the fact that they need to stop drinking booze. 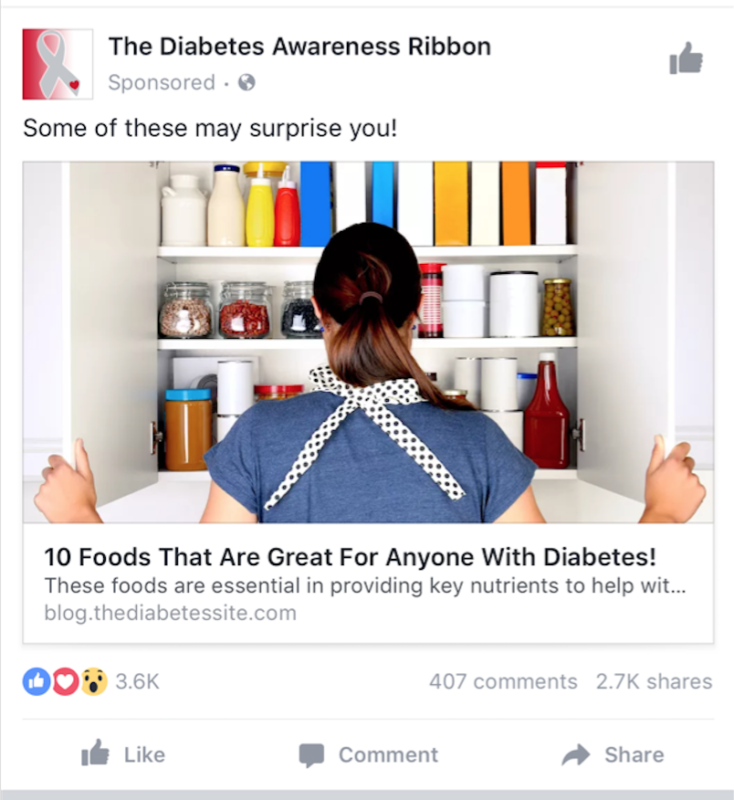
In our quest to avoid the truth and focus on individual super foods that will save us, this post is telling diabetics that dates are so amazing because 7 of them provide 4g of fiber. They forgot to mention that 7 dates equals 126g of carbs with no fat, so that’s pretty much like a syringe of sugar shot directly into your blood if eaten on an empty stomach. None of these top 10 lists had protein, and the only fat was flax seeds (for their omega-3’s) but what about fatty fish or fish oil, which is much more bioavailable? Why aren’t we instead telling them to avoid excess carbohydrates, because the last time I checked, you can actually reduce blood sugar by… not eating sugar!
I’ve been on a protein and meat vindication kick lately, looking into how much protein we need, how much we’re eating, and what the best sources are. For this post, I decided to switch gears and look at the recommendations for carbohydrate intake to see where they came from and if it matches what we’re telling people to eat.
How Many Carbs Do We Really Need?
The short answer: ZERO.
The macronutrient recommendations are based on this book published by the Institutes of Medicine. I reviewed the recommendations for protein intake in this post, where I illustrate that the science justifying the RDA for protein is pretty poor. The evidence is even worse when looking at the carbohydrate recommendations.
Here’s a direct quote:
“The lower limit of dietary carbohydrate compatible with life apparently is zero, provided that adequate amounts of protein and fat are consumed. However, the amount of dietary carbohydrate that provides for optimal health in humans is unknown. There are traditional populations that ingested a high fat, high protein diet containing only a minimal amount of carbohydrate for extended periods of time (Masai), and in some cases for a lifetime after infancy (Alaska and Greenland Natives, Inuits, and Pampas indigenous people) There was no apparent effect on health or longevity. Caucasians eating an essentially carbohydrate-free diet, resembling that of Greenland natives for a year tolerated the diet quite well. However, a detailed modern comparison with populations ingesting the majority of food energy as carbohydrate has never been done.”
They base the carbohydrate requirement of 87g-112 grams per day on the amount of glucose needed to avoid ketosis. They arrived at the number 100g/day to be “the amount sufficient to fuel the central nervous system without having to rely on a partial replacement of glucose by ketoacid,” and then they later say that “it should be recognized that the brain can still receive enough glucose from the metabolism of the glycerol component of fat and from the gluconeogenic amino acids in protein when a very low carbohydrate diet is consumed.” (Meaning, ketosis is NO BIG DEAL. In fact, it’s actually a good thing and is not the same as diabetic ketoacidosis that type 1 diabetics and insulin dependent type 2 diabetics can get.) The RDA of 130g/day was computed by using a CV of 15% based on the variation in brain glucose utilization and doubling it, therefore the the RDA (recommended daily allowance) for carbohydrate is 130% of the EAR (estimated average requirement).
What are the Dangers of Overeating Carbohydrates?
Answer: DIABETES (but they won’t actually say this)
On the DRI (dietary reference intake) guide for carbohydrate intake, the column for “Adverse effects of excessive consumption” states “no defined intake level at which potential adverse effects of total digestible carbohydrate was identified.” WHAT? It also happens to say that the maximal intake of added sugars be limited to providing no more than 25 percent of energy. That’s 125 grams of carbs from sugar on a 2,000 diet. To give some perspective, one 12oz can of coke has 39g of sugar. This means they’re saying for someone eating 2,000 calories, it’s ok to drink more than 3 Cokes a day, (plus other carbs) as long as you eat less meat, less fat, and of course, more whole grains. Is that really what we should be telling people?
According to the Institutes of Medicine, “Published reports disagree about whether a direct link exists between the trend toward increased intakes of sugar and increased rates of obesity… it appears that the effects of increased intakes of total sugars on energy intake are mixed, and the increased intake of added sugars are most often associated with increased energy intake. There is no clear and consistent association between increased intake of added sugars and BMI. Therefore, the above data cannot be used to set a UL (upper limit) for either added or total sugars.” WHAT?!?
I’m not kidding, this is exactly what it says. The authors also go on to say there’s no risk of diabetes from consuming increased amounts of sugars, and they cite this study, saying that it showed that the more sugar one ate, the lower the risk of diabetes. I looked up the paper, and the authors did say that the more sucrose someone ate, the lower the risk of diabetes, but they also said that glucose and fructose intakes were positively associated with diabetes risk. Last time I checked glucose + fructose = sucrose. How does this make sense? The researchers also found significant discrepancies between self-reported diabetes and actual diagnosed rates of the disease (only 64% of those saying they had diabetes actually were diagnosed) and of course we all know that people love to lie on food frequency questionnaires. Is this really the research we’re relying on to form public nutrition guidelines?
Of course there’s actually tons of evidence that increased carbohydrate increases type 2 diabetes, and that reducing sugar and carb intake reduces blood sugar. Pubmed lights up with evidence showing a low-carbohydrate diet is therapeutic in type-2 diabetes.
So, How Many Carbs are We Telling Diabetics to Eat?
Answer: TOO MUCH
If type 2 diabetes is a result of uncontrolled blood sugars, you would think that we should be telling folks to reduce their intake of sugar. Actually, the Clinical Practice Guidelines and Recommendations from the American College of Physicians lists “Oral Pharmacologic Treatment” as the official treatment, not diet counseling. With depression, for example, other non-pharmacologic methods like therapy and exercise are listed. When a type 2 diabetic does meet with a dietitian, we’re telling them to eat more than the RDA.
Even though we have no actual need for carbs at all, and the RDA is 130g/day, the general guideline for adults with diabetes is 45 to 60 grams of carbohydrate per meal, and snacks having 15 to 30 grams of carbs. For the average adult eating 3 meals and 2 snacks a day (recommended) this equals a daily recommended intake of between 165g and 240g of carbs per day.
The most popular way to educate diabetics is “carbohydrate counting.” In this method, one carb serving equals 15 grams of carbs. One serving of carbs could be 4oz fruit, 1 slice of bread, 1/3 cup of rice (that is a VERY small amount of rice), 2 cookies, or a 2 inch square of brownie. Yes, that’s right. No difference between a cookie and a piece of fruit or some rice. It’s advised that protein and fat be consumed with meals, but no guidance is given on quantities or quality, or why this is critical to include. When I was doing my dietetic internship, the sheet below is what the hospital gave me to educate a sick person with type 2 diabetes who had uncontrolled blood sugars. This is directly from the American Nutrition and Dietetic Association. (Sorry for the bad hospital lighting)

If I started the day with this high carb, low protein and low fat breakfast, I’d be a wreck. In fact, before I started eating a lower carb diet, I actually was in metabolic syndrome. I’ve never been overweight, ate a mostly vegetarian, low fat diet full of whole grains like lentils, tofu, slathered in canola oil. I was doing everything right. At the time, if I went more than about 2 hours between eating I would start sweating, have tunnel vision, and was incredibly irritable. The word is “hangry.” I lived this way for over 30 years. When I do a nutrition talk, I always start by describing how I used to feel, and every time, more than half the room nods their heads signifying they too feel this way. Yet, we continue to tell people to eat this way.
We’re Completely Failing Diabetics.
We nutrition experts are miserably failing at preventing and treating folks with diabetes. According to the CDC, 12.6% of Americans have diabetes, costing us $245 billion dollars in direct and indirect medical expenses. I’ve seen the incredible damage diabetes can do to people and it’s pretty ugly. It’s listed as the 7th leading cause of death, but because people don’t really die of “diabetes” but rather die of complications due to diabetes, like kidney failure and cardiovascular disease, the number is likely much higher. The rate is only increasing, especially in countries newly adopting our “heart-healthy” standard American diet. All over the world, people are giving up their healthy traditional diets and are drinking soda instead of water, using canola oil instead of traditional fats, and eating more refined junk foods – oh and it’s not only unhealthy but more expensive to eat this way too.

Why can’t we tell folks who have diabetes the truth: that eating an “everything in moderation,” high carb, low fat and low protein diet will increase your chances of a completely preventable disease (in the case of type 2) that can lead to a very uncomfortable death?
I wish I could still reference the Facebook post from back in October 2016 of a dessert featuring sweetened condensed milk that the American Diabetes Association posted on their facebook page before they removed it. It was classic. All I have is their response:
The American Diabetes Association lists beans as the ideal protein choice. Beans are one of the highest carbohydrate “protein choices” you can make. Should we really be telling them that beans, dates, oats and barley are superfoods, giving the impression that a few magical additions to their diet will fix them?
As a dietitian with some sense, when I see a patient with blood sugar issues, I recommend a low-carb diet, adding more protein and healthy fats as the very first step. There are a handful of people who get it. In this literature review, researchers looked at 12 studies all showing the success of a low-carbohydrate diet had on reducing or eliminating the need for medication in type 2 diabetics.
“The inability of current recommendations to control the epidemic of diabetes, the specific failure of the prevailing low-fat diets to improve obesity, cardiovascular risk, or general health and the persistent reports of some serious side effects of commonly prescribed diabetic medications, in combination with the continued success of low-carbohydrate diets in the treatment of diabetes and metabolic syndrome without significant side effects, point to the need for a reappraisal of dietary guidelines. The benefits of carbohydrate restriction in diabetes are immediate and well documented.”
Why Won’t We Tell Diabetics the Truth?
Answer: The real truth is that sugar, junk food and insulin sells.
Sugar is sexy. Brownies sell magazines and gets clicks on Facebook. Scrambled eggs, plain roasted chicken, or sautéed swiss chard does not. There’s a ton of bias against low carb diets, and a lot of financial interests pushing pharmaceutical intervention instead of a dietary change, and the people who are behind the dietary guidelines are also the ones charged with promoting commodity agriculture (wheat, corn and soy.)
It’s time to admit that we’re failing diabetics.
We can do better. They deserve the truth.
“I use the ‘cigarette’ analogy. We know it is bad to smoke, so we tell patients not to smoke. Why don’t we do the same thing with sugar and processed starches? The excuse I hear is that ‘people won’t stop eating sugar and starches.’ However, by the same analogy, we could have thrown up our hands and said, ‘people can’t give up smoking.'” – University of Alabama at Birmingham Professor of Nutrition Barbara Gower, Ph.D. (one of the authors of the paper quoted above)
Here’s my unsexy truth:


Thanks for writing this. I was diagnosed with type 1 about 4 years ago, did some reading, and immediately adopted a low carb diet. I constantly cringe at recipes declared diabetic friendly. I recently went to a new endocrinologist in order to get a continuous glucose monitor, and literally ended up in a fight with her about the safety of my diet. She thought I should keep my blood sugar higher to avoid the risk of going low. I tried to explain to her that the target blood sugars she was suggesting would be damaging to my body and when your body can use ketones, low blood sugar’s are not nearly as dangerous… I have NEVER had a dangerous low blood sugar incident…. And she said that ketones lead to dka…That’s when I gave up on her.
Good on you Miranda for taking your health into your own hands. How empowering does that feel. I’m not diabetic at least not anymore but I was surely fast approaching it. 2016 I started the Keto way of eating – as a natural evolution from the Paleo way and lost 50+ lbs in 10 months. Keep up the good work Miranda. Robb and everyone else that is helping the world as well! Peace!
All the yes here❤️ I am an RD (10 years now) as well currently working in dialysis. DM is the reason half my patients are here and I so wish that information as you are speaking of could have helped my patients before they got here. When I worked in Outpatient and educated DM patients I taught carb counting bc that it what was shoved down our throats in school 12 years ago. Big box companies represent our organization and we all now research that is put out there is published if it looks to “favor” to support the product. My views have changed over the years after I have grown and become more aware working with patients. I in the last few years have adapted a Paleo way of eating but more so Grain and Dairy free. I feel so much better, energy levels, WT maintenance. I now have changed my education for DM patients to what you are speaking of. Pharmaceutical companies are beyond out of control and empowering patients that they have more control by diet and movement than what they think they do – better outcomes? thank you for this!!
Hey miranda im currently going through the same thing just started my second week of pump training and next week getting cgm. They have assigned me a dietician that is textbook to what this article describes. I argue with them all the time. Its sad doctors don’t want to actually help people cure themselves anymore. The ketogenic diet is what was actually prescribed to diabetics pre 1921 before the discovery of insulin. But now pharmaceuticals can actually make money on insulin so they changed that real quick.
The picture of the diabetic meal plan is borderline criminal when you think about it. 15 carb counts, at 15g/count…for a person whose body can’t properly handle carbohydrates! Good Lord!!
My wife had gestational diabetes with our 2nd child. She was given a similar meal plan and instructed how to count carbs and test her blood glucose. My wife was determined to stay away from insulin and shots. At the same time is when the Primal Blueprint came out [back in the early days] and I was reading about all of this. My wife followed the diet to a “T”, and surprise-surprise, her 1-hr post-meal blood sugars for the first week were all elevated. As we talked through what I was reading, she tried what we learned and everything was great. She even lost a few pounds [which freaked everyone at the office out since she was pregnant]. She brought up to the dietitian how the suggested meal plan had too many carb counts for her and how she had eaten far less in week #2. Rather than be happy she was able to control her blood glucose during week #2, the dietitian was really upset she wasn’t eating enough carb counts and following the plan. We were completed dumbfounded by this.
Being logical and reasonable adults, we did som more research. We quickly decided she had to control the blood glucose and that elevated glucose was bad. We also know the suggested meal plan was a means to the end and we had to focus on the end. So, my wife lied to the dietitian about what she was eating, pretending to eat the recommended carb counts. Since her blood glucose numbers were awesome after going Primal, everything worked out. That was almost 8 years ago and we haven’t looked back.
It should also be noted that my son who she was pregnant with has been lean since day 1. We believe the Primal eating during pregnancy helped “program” him for the better.
Great article!
I wish I would have know more when I had gestational diabetes.
I went to diabetes classes and followed the 15-30-15 rule. I was put on 4 different types of insulin and ended up developing type 2.
I’m now LCHF (low carb/high fat) and went medication free after the first two months (with my doctors approval) went from 9.2 to 7 A1C in 3 months!
Congratulations! Good for you.
I began a LCHF way of eating on March 31, 2015. I brought my a1c from 11.2 to 5.7, literally cutting the number in half. I did this on my own against my endo, pcp and nutritionist recommendation. I told them all that it is criminal the way they suggested I eat !!! I believe that diabetics eating this way and telling the world of their success is the beginning of a revolution in the world of diabetics. Big Pharma and the medical community need to take off the bandaid and begin to save lives. Period !!
What a bunch of nonsense! It’s never, ever healthy to deprive your body from any nutrient. You might feel better on the short term but you’ll slowly wither away on the long run. I know we’re living in the age of fad diets but it’s a dangerous trend that needs to go away. It might work for type 2 people, although I personally know one who doesn’t eat carbs and her sugar results are textbook perfect but she’s getting weaker and weaker and has developed a bunch of complications because guess what! Her cells are still not getting any glucose just like with people whose blood sugar is high because their cells can’t take it up. The results are the same. Please stop spreading this very harmful pseudoscientific misinformation.
What you wrote sounds like nonsense to me. What nutrients are being deprived exactly? You’ll wither away in the long run from doing low carb? That just doesn’t stack up with science and what we see.
Your body breaks down fat and protein into carbs if you need them. Any carbs that are not immediately used in excercise and metabolism are stored as fat until your pancreas can’t handle the load anymore or you become insulin resistant. There is no such thing as a carb free diet if you eat veggies and an occasional fruit. A carb free diet is how diabetes was always treated and successfully until the powers that be started pushing whole grains into the picture and the attitude that a little won’t hurt.
I was of the people that slammed the ADA about that recipe. I’m a reformed type 2 diabetic with a non diabetic a1c from low carb. We are failing diabetics. It’s a tragedy.
Thank you Amanda for ‘slamming the
ADA”. I just don’t understand why they don’t get that high carbs leads to metabolic syndrome that leads to diabetes. Who are these people teaching the dietitians? I just don’t get it. It’s common sense to me. It sure is a tragedy. Thanks to Robb Wolfe and others like him the word is getting out!
Thanks for writing this, I couldn’t agree more. I’ve been wanting to write something similar for quite some time and now I can just share this.
Oh my goodness, yes. As usual Diana, you hit the nail on the head. I’ll be sharing the crap out of this one!
I was diagnosed as an adult type 2 diabetic almost 4 years ago. After a year of trying it the traditional way, my blood sugars were heading out of control, my weight was exploding and I was put on insulin to bring the sugars back down when they got too high.
I started searching online and found 2 groups on Face Book. 1 is a Low Carb/High Fat group, not specifically for diabetics, but supportive of them. The other is a group with the same Low Carb/High Fat standards, but specifically for the needs of type 2 diabetics. It’s from them I found this article.
Doing what they said to do was hard at first. I fought cravings for 2 weeks, but kept faithful. Finally, it became easier. Result? In 3 months my A1C went from 10.5 to 5.8. Yes, I said in 3 months. I also lost almost 50 pounds in the same 3 months.
My mother died shortly after that and my daughter’s family moved in with us right after that. The stress caused me to go back to my habits of emotional eating, but the tools I learned have helped me keep my A1C below 6, even if my weight has been creeping back up again.
My best friend is diabetic, as is her husband. She goes the traditional route, claiming what I am doing is unhealthy. But I am watching their health slowly deteriorate before my eyes, and while I deal with other stress-related stuff (my daughter’s family still lives with us), my endocrine health is great.
Can you share the Facebook link to the group you mentioned…Low Carb/High Fat standards.
Thanks!
I don’t know which one she meant, but I’m in an excellent Facebook group called Reversing Diabetes (just search for “Reversing Diabetes” in FB).
Cathy, please take care of yourself. It is horrible to watch others on the traditional diet and know that they are killing themselves. I have a relative doing just that. The more he eats, the more insulin he takes, and the hungrier he gets, and the more he eats, and the more insulin he needs, and and and….. They are shocked that I won’t eat or drink something because of the carb count. They look at the calorie count and fat grams. I said I don’t care about the calories or fat, just the carb count. Then they say “well it’s only 3% of RDA”. I say I never ever look at or believe that. I also do some intermittent fasting and they are shocked that I rarely get hungry. I have my issues and should lose some weight but I think I am fairly healthy and will continue to be low carb and grain free for a long time.
I have been diabetic type 2 for over 25 years. I figured out many years ago before the Paleo trend that I needed to chart my own way. I figured out over time to cut out all sugar, anything made from flour, potatoes and rice. Moderate protein as it raises blood sugar too although not as much as starch. I eat fruit in moderation. I exercise daily I have stayed free of all complications. The Paleo diet is healthy but is more restricted and quite difficult to maintain for all those except the most motivated. I take no drugs but a small amount of long acting insulin as at 78 years old I don’t make enough insulin. Try my plan and see how you do. You can advance to Paleo is you need to. I don find my diet hard to maintain at all.
When diagnosed with Type II Diabetes in 2004 my GP wrote a script for Glyberide/Diabeta. I said I didn’t want to take it. I asked why she would order a medication before giving me the chance to try diet. She said ‘because no-one sticks to a diabetic diet and most end up on meds including insulin, because it is a progressive disease.” Yes it is progressive because diabetics do follow the prescribed diet – high carb diet! I went to the diabetic teaching and was told to eat a lot of carbs, which I knew was wrong. I did take meds for a while but when she suggested basal insulin and I had a blood sugar of 1.4 mmol/L (26 mg/dL) (with minimal symptoms because I’m on a beta blocker) I decided to get serious.. I started Ideal Protein and on Day 6 I was off my Diabeta with normal blood sugars. That was 5 years ago. I’m following a 98% grain-free low carb diet (98% = occasional cheat) and am doing quite well. A wonderful side effect of being grain-free is that my blood pressure has improved. I’m still on BP meds but off the one that gave me terrible swelling of my lower legs. (Calcium channel blocker). It’s hard to spread the word even to diabetics given the current recommendations of high carbs. It will be an incredible world when dietitians are taught the low carb lifestyle for diabetics. Thanks to technology, the word is getting out. Thank you Robb Wolfe and Diana Rodgers! Robb, I listen to your incredible podcasts all the time.
Oh, and one more crazy comment: I wanted to get a consultation from a (hopefully proactive) local cardiologist. I was told that I should lose 30 pounds and he said to eat a light dinner like soup and a sandwich. It was all I could do not to laugh and tell him what I thought of that. I’d love to have soup and a sandwich but that is not on my diet ie ketogenic. He told me to eat low fat and gave me a pamphlet describing the low fat / low cholesterol way of life. I asked about finding out my LDL particle size and about inflammation. He said he just treats high LDL with statins. He said if I didn’t take my statin, that was my choice and that he’d put me on it after my ‘first event’. (Ie heart attack). I was not a happy patient after that kind of care.
Ours (Canada and USA) is a reactive health care system and getting costlier to consumers / tax payers / insurance companies all the time.
Yes Maryanne, I have been angry and really upset over this very thing for a few months now. I found out about functional medicine because my son was diagnosed with fibromyalgia. A few summits and several hundred hours of research later, it became apparent just how little common sense is present when it comes to how are health care cares for our people. It makes no sense to do a couple of tests and then the patients has to keep coming back dozens of times to run more tests. (What? you thought that my being bedridden for 2 years would go away on its own in between visits?) Meanwhile, each visit costs the taxpayers more and more money. Furthermore, the health care system accepts final diagnoses of things like fibromyalgia thereby rendering the patient a victim. One lady was diagnosed and it turns out (after many doctors) she had severe heavy metal toxicity and a few other things. Once those were addressed, she was perfectly normal. In my son’s case, they simply aren’t doing all of the necessary tests and the way one of them is done makes no sense based on how a naturopath had it done previously. So, should the government spend a few thousand on the necessary testing to completely assess the patient possibly (probability of 67% recovery from fibromyalgia) bringing them back to complete health? Or should the patient be restricted to substandard tests and care due to financial hardship (can’t afford a functional doctor) thereby leaving the government to pay disability for the rest of the patient’s life?Let’s not forget the additional costs of secondary diseases like heart attacks that send one to emergency because someone who is suffering can’t get out of the house for long periods of time or exercise because of their illness? A province’s or state’s tax dollars is divided up in portions to certain interests including health care, but wouldn’t flexibility make more sense? My son would sooner be healthy and thriving than what they are doing for him now. It’s so disappointing. I’m just glad I found out all of this when I did and that I kept an open mind. Otherwise, I could have ended up like my entire paternal relatives’ side who all died with severe type 2 including amputation.
The reason diabetics should not consume foods high in saturated fat such as meat and butter is because this will increase your body’s production of low density cholesterol (bad cholesterol). This bad cholestorol blocks your arteries with plaque it creates. The single best diet to go on is a fully plant based diet. This diet has been found to even reverse type 2 diabetes. Meat is the last thing you want to consume for a healthy, long lasting life. Humans should make meat no more than 10 percent of their daily diet. Please try a plant based diet for just two weeks and see if you find any changes. I guarantee you will.
I went Vegetarian for 4 weeks and my numbers went the opposite direction. So no it does not work going strictly on a plant based diet.
But what about a 25 year vegan–> vegetarian –> pescetarian. My husband was just diagnosed with DM after all that. We eat out on average once or twice a month. We cook most everything, but our diet is very carb heavy. That’s how we eat to not feel like we’re starved. It hasn’t worked for him unfortunately. Add in a drop in physical activity with his being a stay at home dad or baby/toddler. Not even any weight gain (he’s overweight but stable). You don’t find a lot of information out there about vegetarians who become diabetic. But now I’m researching options for a change in diet as he’s miserable even trying to stick with the recommended carb intake for diabetics! It’s really conflicts with out ethics and environmental outlook as we’ve always considered vegetarianism good for the body and good for the planet compared to eating meat. Hopefully we can find a balance that works for us and promotes his health and our ethics.
Sarah,
You are incorrect. This is the lipid hypothesis, which has been amply debunked and was a product of bad (corrupt) science to begin with.
Blah blah blah.
No matter what the evidence.
Did you know (apparently not) that sat fats INCREASE HDL’s?
My diet, long term, is about 4:2:1 Sat/Mono/PolyUn. My lipid panels and related ratios are to kill for. Age 72.
Plenty of meat, dairy, eggs. Some vegetable matter, some carbs, both low.
I just started my no carb diet and wOw..and just for one day my blood sugar shoots down to normal.
What were your meals? Almost everything, even veggies have carbs.
I am on a 24 hour fast and in the last five days have lost 5 lbs. Instead of taking 50 units of Lantus I am now down to taking only 15 units. I remember when I was first diagnosed as a diabetic the doctor said come back in every month and we can measure your BS. I said NO. I need a meter. I immediately changed my PCP. Honest, these MD’s don’t understand what diabetics need to be doing to lower their blood sugars and……….with the possibility of actually getting off of insulin forever. It is going to be fun to say to my doctor: I am cured and I did it myself.
I’ve been saying this for 20 years but I’m apparently just crazy, according to most people. I’m an RN and it used to boil my blood to have serve the “diabetic tray” to the patients when I was working in hospitals. Mashed potato with margarine, tiny piece of meat, sweet corn, dessert and a whole wheat roll. UGH! I’ve been diabetic for over 20 years and have been eating some form of low-carb off and on for about 18 years. My HgbA1c has been around 5.5 for the past 5 years since I started eating a lower-carb Paleo/whole foods approach and have gone from needing 2 oral diabetes meds and an injectible (Byetta) to only very low dose metformin. It’s terrible, but each time I’ve had to change clinics/health care providers, I’m forced to attend a ridiculous Diabetes Education session during which I’ve learned to mostly keep my mouth shut. I always tell the truth about what I eat, and my lab results and how I feel speak for themselves, so when they try to steer me towards that “everything in moderation, more whole grains” crap, I just say, “that’s ok, I’ll just continue what I’m doing, thanks.” I particularly think of those RD’s when I’m eating coconut oil out the jar with a spoon. LOL
The entire Nutritional Therapy Association would agree with you. This is what they teach their students in nutritional therapy. There is intelligent help out there, if you’re willing to get a REAL second opinion.
Best article I’ve read in a long time…and spot on!!! My sister and I have both adopted a Ketogenic lifestyle. Blood sugar issues run in our family, she had gestational diabetes and was borderline type 2, I have hypoglycemia and my dad has type 2. She has lost 50 lbs. since July, I’m so happy she is taking her health serious, she was never one to care much before but I think not so great blood test results were enough to kick her in the butt! My dad had 2 strokes a couple years ago, I believe it was due to prolonged high blood sugar. I was floored when the dietitian (not what I would call her) came to talk to him in the hospital and she was telling him he could have 45 grams of carbs a day, whole grain toast, potatoes, rice!! I also have had bad info given to me by a nutritionist, knowing I have hypoglycemia the nutritional guideline she gave me was 3 times as many carbs (whole grains) as I ingest now, and those are all from vegetables! Also, with a history of Alzheimer’s in our family, a LCHF diet is the best thing for us…now if I can just get my kids to quit asking for dessert and “real” syrup!!
27 years ago when I was diagnosed with type 1, I remember the dietitian warning me against eating vegetables. She said they were too full of carbs to eat them regularly. I was brainwashed by the recommended diet.
So glad I switched to low carb. My A1C has not gone above 5.9, and I now take 1/3 of the insulin I used to take.
This is extremely offensive in that you have completely and totally IGNORED the fact that type 1 diabetics exist!! We NEED carbohydrates in the form of fast acting sugars in order to SAVE THEIR LIVES in the case of low blood sugar or hypoglycemia!!! Only a complete quack would ignore the huge difference between type 1 and type 2 diabetics, and have NO BUSINESS GIVING PEOPLE MEDICAL ADVICE THAT COULD KILL THEM!
Low carb works really well for type 1s as well. I did make the distinction. There are several comments on here from type 1s about how they were able to lower their A1c with a better diet.
Yes you did discern the difference between T1D and T2D and yes LC can help tremendously with T1D. However, what you fail to clearly distinguish is the fact that T2D, (dysfunctional pancreas) can actually be reversed as an illness, whereas with T1D this food regime is only an aid for insulin management… in particular regard to reducing and minimising the use of insulin… ie: minimising the impact of T1D on lifestyle.
In this light there needs to be a very very different discussion when it comes to LCHF and T1D.
You see,… T1D , as you well know, is a breakdown failure of the pancreas and non-production of insulin. So… in this sense many T1Ds see this as a ‘fait accommpli’, and that dosing insulin is the remedy..
The notion of LCs doesn’t sit right with many T1Ds because they have been needing to deal with the lack of any insulin in their bodies and also the unpredictable potential fluctuation of BGLs influenced not only by food, but also by stress, activity, emotions, environment, antibiotics, work, malfunctioning devices, insulin resistance,… and of course insulin itself.
There is a huge difference between the impact of diabetes on those too different group categories.
What you also fail to embrace is that many many people in the T1D community are of the belief than increasing insulin can stabilise BGLs irrespective of food intake. So for many people the issue of food intake and especially LCHF is not truly their main preoccupation. Their focus is more on the managing the unpredictability of the illness.
Sure LCHF does help in optimising the the body’s health in providing the best conditions for stable BGLs but unfortunately that is not the only preoccupying factor for T1Ds when other external influences play a huge role.
The bottom line is the missing link…
Nutritionists seem to focus too much on ‘food’ and T1Ds, and especially their medics, tend to focus too much on insulin.
Somehow if nutritionists could bridge that gap and T1Ds/medics could bridge that gap.. there may be a more convincing argument for LCHF regimes.
As a parent who has nurtured a child dx@22mths of age in 1999, I have a world of experience with whole food approaches and developmental stages of physical growth of my child. I have always found that the biggest hurdle to overcome is convincing T1D parents that T1D IS actually an illness related to gut and food issues.
Perhaps as a qualified nutritionist you could look at this perspective and incorporate into the broader framework of discussion.
So, your initial complaint is that I did not discern the difference between type 1 and type 2, but now you are saying I did. By the way, I love the tone. Super constructive and makes me really want to engage with you and sympathize with your position. But I’ll engage anyway…
Welp, as you say, I’m a nutritionist and my concern is food. As you say also, “Sure LCHF does help in optimising the the body’s health in providing the best conditions for stable BGLs but unfortunately that is not the only preoccupying factor for T1Ds when other external influences play a huge role.” So, of course, because food can optimize health, this is my objective. I’m not really sure what you’re expecting I should be doing – of course I council people on how to adjust insulin when reducing carbs. Are you saying that I don’t address this in my clinical practice? Insulin is NOT GOOD in excess, and you can reduce your A1c with a better diet, so why not be open and not offended when someone suggests that all of the sugary foods, and advice that diabetics should be eating over 250g of carbs a day is probably not a good idea? Are you actually a fan of these diabetes magazines with cakes on the cover? Is this the right message in your mind?
First of all .. I am not the original poster of that comment. That was Diane.
Second… u fortunate that you have interpreted my points as ‘on the offence’.
To the contrary.
Sad too that misinterpreted my tone. I believe I was being quite pragmatic in my comments and simply providing a broader scheme to the topic rather than the seeming narrow parameter of discussion.
I have not suggested anything in regard to your personal practice as a nutritionist not at all… In fact I am all in favour of what you are practising and the regime you advocate.
I personally am against all that you have mentioned about current medical advice and diabetic marketing of course.
I have nurtured a T1D from babyhood to adulthood
With whole foods and low carb intake.
What I’m trying to say is that first you need to convince people that T1D … IS … about food and gut.
Most T1D parent /caters are not in this mental framework and on diagnosis of their children the medics do NOT focus on this at all. The focus is purely on carb counting and matching insulin. …especially with ‘pumping’. Most people are taught to eat what they want and adjust the insulin accordingly. This is what is being taught and this seems to suit people who are either non caring/ in knowledgeable about food or people who are simply struggling with the angst of diagnosis, especially parents of young children.
What I was trying to help you understand that more than often especially with T1D parent/carers, it is the mind of these people that you have to influence.. to change their perspective that T1D ‘is’ about food not only about insulin.
That is the bigger hurdle.
That is why I suggested that there should be a completely separate discussion topic and focus for T1D.
Discussion including both Types of diabetes always goes askew and often evoke anger and defensiveness amongst the T1D community.
That is the reality.
I just feel that nutritionists need to embrace the broader influences of the illness in their approach to convert people to LCHF.
Believe me, I am part of the community and it can be a very antagonist environment at times.
Perents have a lot to give as input.
I hope you understand where I’m coming from a little more explicitly. Apologies if I have come across as negative.
Diane,
Your criticism is just silly. Type 1 diabetics also occasionally need glucagon, and she didn’t mention that either, but that doesn’t mean her article is invalid.
T1s (and T2s) DO NOT need a high carb diet, and are greatly helped by low carb diets, which was her point.
I have type 1. Had it for 29 years. We do NOT need fast acting carbs to save our lives ! That can be done with glucose tablets or gel on an as-needed basis. And if we eat a low carb diet we can reduce the insulin needed and therefore reduce the need for glucose tablets to resolve any instances of hypoglycemia. This was an EXCELLENT article for T1D (and presumably T2) and you can find a number of similar articles (and believers) online. I was first turned on to the low carb diet by Dr. Richard Bernstein’s book – The Diabetes Solution and continue to search for and read articles like this to improve my knowledge. My A1C on a low carb diet is 5.7 and I’m working to lower it. Prior to the low carb diet, my A1C was in the mid to upper 7’s.
Actually, there is an elder doctor with type 1 who eats a high vegetable, high meat, no fruit or carbs diet and he’s still kicking at 78 years. (last I checked) His name is Dr Bernstein and I’m sure that Rob Wolf knows who he is. I don’t know of many with type 1 who are still alive at that age. He doesn’t believe in the HF part but that’s ok. The point is that he doesn’t use carbs or sugar. You can check out his site here: http://www.diabetes-book.com/diabetes-diet/
He also has a 1 hour teleseminar webcast coming up on April 26, 2017 that you can register for.
If I don’t eat a lot of veggies(fresh)/legumes/oatmeal every day, I get horrible edema and constipation. I eat just a little meat with fat, no processed food. (usually) I have never had high sugar and don’t wanna have it.
??! You say ‘never had high blood sugar’ like it’s a success (which it is) — but then say if you don’t eat a specific diet you get edema and constipation?! That you have to ‘manage what you eat’ to avoid those is ALSO symptomatic of a screwed up diet! Please keep researching. Please studying paleo and low carb high fat more closely, to make sure you’re doing it right. If you have to “force” your body to do (or not do) what it would normally do if healthy, it means you’re not there yet!
I lost 60 pounds 5 years ago on a low carb diet (Atkins) and have gained half of it back. Am going back to low carb in 2017 looking forward to reaching that point again where eating processed sugar rich treats were gross to my taste buds.
Thank you for this post. It’s often overwhelming trying to figure out what foods are best when you’re diabetic. Common sense has always told me that a lot of what is recommended by HCPs is not ideal. If I ate that recommended breakfast on your printout I would probably have one of the highest blood glucose level of my entire life! Banana, cereal, and bread, but no protein?! I would be asleep on the couch with drool running down my chin if I ate that.
I’ve done pretty well with my type 2 diabetes by trial and error. I was diagnosed at 26 when pregnant with my first child. Thirteen years later, and after experiencing my highest A1c at 7.6 last year, I’m working on more diet changes with the help of information like in this post. I’m down to 6.9 already. That ugly A1c along with the handful of pills I take daily at 39 years old, and watching my mother die at 65 from complications of diabetes have been huge motivators for me. Could you possibly point me toward any other information you think would be helpful?
Lelia, you might want to see Dr. Fung’s web site, Intensive Dietary Management at https://intensivedietarymanagement.com/blog/
Also check out Dr. Bernstein and the Diet Doctor.
Excellent post, thanks Diana! Years ago while in a doctor’s office for an FAA medical exam I picked up a magazine for diabetics in the waiting room. I could not believe my eyes, recipe after recipe of sugar-laden sweets. WTF! I used to eat my eggs on toast for breakfast. Two hours later I’d be starving and light-headed upon standing up. Ditched the bread, now eat my eggs on greens sauteed in plenty of fat. No more hypoglycemia!
BULL! til you walk in those shoes…literally, as a person with gout…i eat No protein besides milk products and eggs… i get along much better…good luck to ya!
This was not a post on how to manage gout.
diagnosed four years ago as type 2. two months ago I was on 80 units of insulin and x2 metformin a day.
it was not working so the doc tells me I need to stop the metformin and start a weekly injection plus the 80units. my BS was almost 200 a lot of days.
really no consoling on diet.
well that was going to cost me 500.00 per month plus the insurance.
happened upon a youtube vid. about low carb diet and diabetes. I decided to try it. two months now, I have lost quite a bit of weight and as of yesterday BS was 96 and this morning 111. I went off all medication a month ago.I allow myself about 30 to 40 carbs a day. I won’t go back to eating just anything and am trying to get my wife to give up her junk food.very high carbs.soda’s,potato chips, candy and stuff. she lives off it.she has diabetes in her family{dad} history and her brother has been diagnosed. I did not.
Milk products and eggs — two foods that are VERY high on the list of things folks can be over-reactive to! Gout is also a clear sign that you’re not eating right. Please keep researching!
I often wondered about the Mid-West Pot Lucks that I went to that had Angle Food Cake with strawberries in syrup set aside for the diabetics. Ha! That is all carbs but no/low fat. Someone started that a long time ago and NO ONE would listen to me that is was completely wrong.
Great job. I met my diabetic specialist 4 weeks ago and he told me not to come back until I had diabetes again. I was on 120U fast insulin and 120U slow (basal) a day. I went on a hi fat lo carb diet + 30mins walking a day 5 months ago. I’ve lost 25kg (55lbs) take no insulin (only metformin) and have an A1c of 5.4 (was 12.3). This article is spot on.
I have had Type 2 for over 20 years and was following the recommended diabetic/Canadian Food Guide for diabetics. At the onset, Metformin was prescribed. Years passed and that was enough, so I was prescribed Insulin, and found I was allergic to it, not sensitive, but allergic, causing hives and eventually the start of a seizure, and had to cease taking it. So still following the recommended diet, and with dieticians and Doctors having no further advice for 2 years, during which I developed nerve damage in my legs and feet. So since what I was doing was not working, I switched to a gluten free, very low sugar, low carb, high protein life and began walking a minimum of 1 full hour every day. I have now achieved what my Doctor calls “controlled diabetes” and was even able to reduce my dependency on the recommended diabetic drug. The additional benefit was that I lost 75 pounds in a year, easily and enjoyably, by doing what you advocate and not what had been recommended and still recommended by other ‘specialist’.
Thanks for the straight talk about this! I’ve been uncontrolled for the past three years and the doctor just keeps throwing more medicine at it…..during this whole time I’ve been attending and following (for the most part) the recommended diet as layed out by two dieticians. Not as active as I should be though. But high blood sugars are my norm now I’m getting tingling in my feet and hands and my eyes are bothering me.
I recently attended an all day diabetes education class and was so disillusioned by their recommendations that I didn’t even go back for my follow up appointments. The presenters, one of whom was a grossly obese Type 1 diabetic, were passionate and obviously wanted to help people but they were following the guidelines listed in this article. The normal weight presenter mentioned that the obese presenter did an “excellent” job of monitoring and controlling his blood sugar but he was shaky in both the morning and afternoon sessions and admitted that his BG level was in the 300’s that day!! How does a Type 1 become obese? I don’t know for sure but from what I learned, it seems he would have to be injecting tremendous amounts of insulin and the only reason to injest tremendous amounts of insulin is because he’s eating tremendous amounts of carbs, just as the ADA prescribes.
Hi everyone. Loved your article! Not a diabetic but diagnosed with PCOS and so have raised everything due to hormone imbalances. Curious if this would help balance out my endocrine levels. Thanks all!
Yes it will. 🙂 My story was recently featured on Diet Doctor. My fertility was completely restored with LCHF. https://www.dietdoctor.com/low-carb/pregnancy
To throw in another case study: by switching to low carb and intermittent fasting, I lost 75 pounds, trimmed 8 inches off my waist and got my A`C from above 9 to under 6, while quitting Metformin in the process. Just by eating the right food in the right timing pattern.
How unfortunate that going against the conventional “eat carbs and eat frequently” advice is considered radical and controversial!
I have been a No 1 diabetic for 3 years. I have been encouraged to find my health status by eating ‘half vegetables, quarter carbo’s and quarter protein’. Reduce my weight to what it should be. Exercise responsibly and enjoy life to the fullest. I have reached 70 years of age. The diabetic clinic has been so helpful warning me of issues if I do not keep living according to a healthy plan. So far good. I thank the health professionals for their care of me and encourage others with ‘our’ conditions to do the same. Take responsibility for our issues.
Interesting and informative, yet not sure an entire profession had to be thrown under the bus to make your point. A vast majority of RDs do not follow the dated recommendations you describe here. Many take it upon themselves to learn and know better. It is all so personal to the individual and the RD is trained to work with the individual and do all that is necessary to decrease carb and increase protein and fat. Your article makes it sound like everybody with diabetes is up for that. You know damn well, they are not always receptive and the RD is trained to get them there. Patient, diligent, empathetic… foreright, truthful… the message remains clear, go after the carb intake, it is the problem… individuals with diabetes in America with its plentiful sources of carbs at every turn, must be supported and encouraged to go low carb… RDs do that, please don’t generalize! I’m quite sure your education covered that.
Actually I was not “trained” to go after carb intake. I was trained “everything in moderation” and that we need to reduce overall calories. The handout I show is from AND. It’s completely irresponsible to tell someone with a carb intolerance to eat that for breakfast. I need to generalize based on the climate that’s out there – from the top down. The USDA, the AND and the American Diabetes Association all have very similar recommendations. Of course there are anomalies and it sounds like you’re one of them. I’m also part of a Facebook group of progressive dietitians that believe in lower carbs and real food. We are the exception, not the rule.
As a fellow low carb dietitian, curious about the Facebook group you’re a part of? Love this article! I’ve been telling my patients to follow a low carb diet for the last few years and your story sounds similar to mine. I’ve recovered from living in a constant state of hangry!
friend me on Facebook and I’ll connect you. It’s a private group for paleo/real food dietitians, and there are lots of us!
Same here, I’d love to connect!
I’m a pharmacist and would like to maybe be part of the FB group if you’ll have me. We can chat more through their if you’d like.
I’m a type 2 diabetic, diagnosed 3 years ago with metabolic syndrome. Metformin didn’t suit me so I’ve been eating the LCHF (keto) way for 3 years now. I’ve lost 2 stones, cured my fatty liver.. reduced from a reading of 185 to 35 and I’ve never felt better. My diabetic glucose readings are now nearly in the normal range.
The sad thing is I had always followed to so called “good advice” low fat and calories which I now believe was what actually caused my problems
Type 1 since 1968. Carb restriction was how I began my D-life as that was standard practice. Rare were meals of spaghetti, rice or potatoes (thank goodness!). Somewhere in the 80’s I quit paying ANY attention to ADA or JDRF. Everything about diabetes is easier once sugar and starch are eliminated and a little fat is added (seriously folks, play around with butter – it acts like an anchor holding BG stable for hours). Perfect health 49 years post dx. Brilliant article – bravo!
Loved the article! I just wanted to say, if 100 grams of carbs – not sugars, carbs – were the recommendation it would probably be great. I recently used a macro counter to see how many carbs I was getting and when I included all the cauliflower, kale and the apple or two I was surprised to see I was usually right around 100! 100 grams of carbs is not really that much, if you include EVERYTHING you’re eating in the counting. I shudder to think how many carbs are actually in that sample menu. My guess: 200+
It really is criminal. I notice it every time I go to the drug store to pick up a prescription: all the diabetes lifestyle products right next to a display full of double-stuff OREOs. So sad and cynical. And so-called nutritionists who cannot think beyond fruit and whole grains. Really? That’s the best you can come up with? They think protein and fat are dirty words. Thank you for calling this out Diana. The Diabetes magazine covers really say it all don’t they??
Here is the answer to your question as of why.
Depopulation through food among other things like vaccines, pharmaceuticals, etc..
But all the evidence is there, you just have to connect the dots. And just like clock work who will be the first to call me a conspiracy theorist?
My comment was censored. Why, probobly because I speak the truth and the truth hurts.
You mean your comment about depopulation? It’s on here. Easy with the attitude fella.
If yo want the truth about how many carbs a day we need….look up Dr. John McDougall. He has his own website, and numerous books about why the body does need carbs….(It’s the way we were created). He has lots of books and cookbooks available too, as well as a FB group called McDougall Friends, as well as his own page.
His work couldn’t be further away from what I’m saying in this post.
You are completely right. I once sent an email to a diabetes educational teacher with this link to a journal stating that a low carb diet is prefered over a highcarb diet for people with diebetes and in some cases can reverse the symptoms completely.
http://www.nutritionjrnl.com/article/S0899-9007(14)00332-3/fulltext
thats the link i sent her. She then flung me back a link herself haha…. you wont believe what she sent back, to this day i still dont think she ever had a look at the journal i sent her.
http://www.eatforhealth.gov.au/guidelines/australian-guide-healthy-eating
anyway i just made this comment to let you know that im glad you getting this information out there, i have family members with type2 diebetes and i believe its a preventable disease.
HI Diana, I would love clarification on one point that I don’t think any of the Type 1’s have brought up in the comments (if they have and I missed it I apologize.) What about the glycogen stores in our liver, that bail us Type 1’s out when we have a seizure due to overly low blood sugar? (this is not a frequent occurrence obviously, and usually can be contributed to an incorrect pump calculation at this point in my life.) Anyhow, for years we’ve been told you have to have some carbs to keep your glycogen stores up. (Albeit by the same people who want us to eat 200+ carbs a day…) Can glycogen be created from fat instead? If so, is there a “danger period” while converting from carbs to fat, where you may be low on glycogen?
As someone who has had plenty of seizures in my life, that’s obviously something I think about. I also have major adrenal fatigue and am hypothyroid, both things that even the Paleo folk are saying require a certain amount of carbs. I eat the Autoimmune Protocol and get about 100 grams carb/day (including all the veggies which are mainly cruciferous, no starchy veggies, and two to three servings of fruit a day).
That being said, if I can reduce my insulin even more I’m all about that…I just haven’t seen anyone address that glycogen thing yet and would love the input of someone that knows about it. I have had more than one friend with Type 1 die due to seizures and no glycogen to save them…so it’s always on the front of my mind. Thank you!
The best resource for learning how a type 1 can reduce insulin/go low carb is here: http://www.diabetes-warrior.net
The book is written by, and apparently for, TYPE 2 diabetics.
Can you explain why you recommend it for type 1s?
I think about that ALL THE TIME! As an RD and recipe developer I always get inquiries for “diabetes-friendly” recipes – I’m careful to suggest meat and vegetables, as much real food as possible. I used to have teach women with Gestational Diabetes carbohydrate counting when I worked at WIC (first job) and I just couldn’t bare it because the more research I did the more I knew it was wrong. The everything in moderation approach works for some situations, but definitely not all – diabetes and PCOS are two prime examples! Great article!
T1D, absence of insulin production, requires refined, exquisite management for health. What is now considered T2D, “adult onset”, could more accurately be called “hyperinsulinemia with insulin resistance” and it’s healthy management has been compromised by using insulin to lower high BG. The resulting high blood glucose #’s in each situation are caused by different processes.
Thanks totally agree. I’ve been Type 1 for 4+ years now and amazed at how many other diabetics I know that just dial up the insulin. I’ve been able to do very well eliminating grains, gluten and getting exercise with just small amounts of Lantus alone – though obviously some days are better. I think the problem in America is that we don’t like tough answers to tough questions – we want the easy way out – or certainly the doctors feel that way and then bow down to the food and pharma lobby.
Great article! As T1D for 51 years, I’m alive and not totally blind because I found the low carb, high fat diet 15 years ago.
It is true that sugar, junk food and insulin sells. It is also true that the USDA promotes wheat, corn and soy and thus have not been able to say that certain people should not eat them. But there is a group that helps promote the advise that a third to half of the foods diabetics eat should contain lots of sugar/carbohydrates. Academics and doctors are the other group. These professors are protecting their egos, their repetitions, their books, their “peer reviewed” articles, their seats on broads, their payola from the sugar industry, etc. All this stuff, of course, protects their jobs and income.
Actually, I am not too angry with the junk food and sugar industries nor the pharmaceutical companies. And, I’m rather neutral about the politicians and the USDA. But the doctors, dietitians and professors should all be sued and then tarred and feathered and then fed only cocoa puffs with fat free chocolate milk until they apologize.
My son has been a type 1 for 2 years now. We have recently switched over to a much lower carb diet (for him as well as to benefit my overweight daughter). I belong to a few diabetes pages for parents. It’s sad that if you ask about low carbs you are pretty much chastised because it’s always “kid first, diabetes second”. It’s okay to let them eat pizza, chips, ice cream, etc, just calculate insulin because you don’t want them to feel bad or different because you changed their diet. My son eats something sugary, doses the appropriate amount of insulin and his blood sugar still shoots up and takes a long while to come down, and then he’s starving on top of that. He is 15 so I think he is beginning to see that lowering carbs stabilizes how blood sugar. We are doing it as a family and not singling him out and putting him on a special diet. I just with the diabetic communities we belong to wouldn’t preach high carbs.
What a wonderful common sense article!
Imagine Diana applying for a job at the ADA.
First question:
“What do you believe is best diet for Type 2 diabetics?”
“A high-fat, very low-carb diet.”
“It was good meeting you. Have a nice day.”
Thank you Diana for a great post, and I wholeheartedly agree! I do think we’re failing people with diabetes, and the general public at large with our current dietary guidelines that are causing type 2. It horrifies me how many people are getting sicker and sicker every day because they do exactly what their doctors tell them to. 🙁
My greatest hope is that all of the diabetes associations around the world will do a 180 on their dietary recommendations like the Heart & Stroke Foundation Canada did recently. They did a webinar where they have said “oops, we were wrong. Don’t cut the fat, cut the crap”. Honestly I cried when I listened to the webinar, I could have written it, I’ve been saying all of this stuff for years!
If you’d like to watch the webinar, I’ve linked it in this blog post of mine. http://rebaweber.ca/service/blog/2017/01/01/this-is-even-huger
Hi Diana. I just wanted to say that I loved this article. You speak the truth. I’ve been on my own journey for the past 5 years after my doctor said that I was pre-diabetic, overweight and recommended that I don’t eat butter, coconut or eggs due to the fat content. I sought a second opinion from another doctor who had a more Paleo approach. He suggested that eggs, butter and coconut should be a part of my daily life. Ha! Under his care, I lost 40 lbs and my blood sugar is perfect. Every meal I fill my plate 2/3 with veg. a palm sized amount of protein, a bit of fat and maybe a few blueberries. My plate was full and I lost weight. I try to maintain an 80% paleo lifestyle and this has worked for me. Keep up the good work.
Stuff like this drives me insane! Don’t even get me started on dates! As a former long time vegetarian, sometimes vegan, dates were my downfall. I went through a raw vegan phase (which is ultimately what let me to primal/paleo/real food/eating to look and feel amazing) where I was anxious all the time (no wonder…my brain wasn’t getting enough saturated fat) I would eat dates like they were going out of style, and feel even more wired. Yeah, I would feel like complete crap on that sample diabetic menu. Today I’ve had coconut oil in my coffee, eggs, lots of greens, salmon and some avocado oil mayo. Oh, and some 90% chocolate. Everything tasted great and I feel amazing. Focused and energetic.
Thanks! I agree. I’ve had T1D for 25 years. Mornings are ESPECIALLY difficult because of a common thing called dawn phenomenon. I had maybe a half cup of blueberries w my breakfast today and it sent my BG skyrocketing. I WISH I could use dates as a sweetener, but as you pointed out, just because something has other health benefits, it doesn’t mean that it will help a diabetic reach their bg goals. I used to wonder what was wrong with me when following what I thought was a “healthy” diet, but was really just SAD.
Thanks! I agree. I’ve had T1D for 25 years. Mornings are ESPECIALLY difficult because of a common thing called dawn phenomenon. I had maybe a half cup of blueberries w my breakfast today and it sent my BG skyrocketing. I WISH I could use dates as a sweetener, but as you pointed out, just because something has other health benefits, it doesn’t mean that it will help a diabetic reach their bg goals. I used to wonder what was wrong with me when following what I thought was a “healthy” diet, but was really just SAD.
I was in a “diabetes friendly” cookoff/recipe competition sponsored by Southside Diabetes in Chicago recently and was a little disappointed at some of the stuff that was touted as “diabetic friendly”.
Really enjoyed this article & comments.
Finding this site probably just saved my life-
Articles like this one are the reason I don’t trust anyone with an RD or CDE after their name. If you are going to label any article as “click bait,” please label this one first. I have Type 1 diabetes diagnosed at age 63. I tried ever diet, including the extreme low carb diet, and was physically miserable and exhausted. In desperation, I joined a whole food plant based very low fat coaching program, @mastering diabetes. It saved my life and sanity. I have GREAT blood glucose control (with a CGM to prove it), cut both my basal and bolus insulins in half, am never hungry. I look and feel better than I have since my 40s. Your recommendations are no better than the shelf of processed chemical laden “foods” the first CDE showed me just before my first doctor failed to detect the symptoms of DKA. Does a low carb, high fat diet work for some people. Sure. Unfortunately, that dirt is nutritients deficient. I’ll take my fruits & vegetables any day. My endo, PCP, and cardiologist ALL agree.
You are so right! There is one doctor that i know of, Dr Richard Bernstein – a type I diabetic – who’s been following a keto-type diet for years and guess what? he’s healthy and almost – if not over – 80 years old, when life expectancy for diabetics never gives those numbers…
Did anybody ever tell you that the major source for fuel for the bodies cells is pure glucose. That fat can be used but it isn’t the prime energy.
Your biochemistry is either really out of date…or, well, yea.
I’ve spent 40 of 50 years drinking, smoking, and eating horrible. I found HFLC, so I dropped 65 lbs, I still drank and smoke and then boom, Heart attack, 100% blockage. Got me a Stent. Okay now what, more Nutrition. I too was handed a flyer called the DASH diet, which I thought was gold like the Food Pyramid I have been LIED to about since the 60’s.
Regardless I wasn’t going to be doing DAPT and feeling bed-ridden in inflammation pain taking a statin wrecking my lower body–if not my heart too. I got several books wheat belly, Dr Davis and others. I researched each drug, I resented not having GRAPEFRUIT.
I went through some dark times, fighting about food with family, but I have come out the other side. I have great BP and no pain, I have reversed everything by DIET and a few supplements. My diet every day I eat some Carrot, Beet, and Apple. I won’t say today a WHOLE one. Eat a Little if you have HEART problems. (different than diabetics, I could be diagnosed as diabetic I guess as I had high BP, but that is no longer true.) When I had my High BP, I thought I was going to die in about 5 years, my vision was going, my mind was going everything out of breath. I just quit everything after I got out of the hospital with the stent. No smoking, drinking. Here I am it’s 2 years now. I feel BETTER than I did say from my 40’s to 50’s
Today this list for ME is: Magnesium Citrate, D3 5000iu, MK-7, melatonin, Krill, liquid coq10 and (lipo C–by the way I FEEL is the measurement) I also will go through other weird things once in awhile like say a Bottle of NIacin, or a Bottle of B1 or ya know, whatever.. I will work it in.
Also I can SWALLOW the pills now. As a smoker I had horrible time swallowing big pills. The apple, beet and carrot are RAW, you eat them RAW. Now I @54 have to FOCUS on my Teeth as I saw a friend DIE cause they couldn’t EAT cause their Teeth were bad at 97yrs. Trust me you want to have some damn teeth if you live that long!! Yeah I see these things changing when HANDCUFFS come out.
Karl has much to say about this kind of diet. He’s right in there with all the other Cardiologists I studied. The only thing I differ is I have a HEART I am caring for, so I eat the Carrot, Beet and Apple EVERY DAY. but I
have also learned to eat LESS. I think many problems could be solved simply by visualizing smaller PORTION SIZES of whatever the heck is on your fork, which you can not out run. ( I work with CEMENT and SHOVELS and digging okay. I would call it toning, you want toning and to exercise ALL of your muscles)
market-ticker.org/akcs-www?post=231890
So I notice many articles say the Doctors had nutrition in Doctor School, but then they just TOSS it all out the window in the field. That’s true, I had to GO AGAINST my cardiologist and the nurse practitioner to get well. I would be on that DAPT stuff still, who among most normal people have the GUTS to go against what their DOCTOR tells them?! seriously. Only a few escape this madness. I couldn’t wait to stop going to the hospital myself.
I also now have gotten another family member OFF their Statin! Funny that I almost destroyed the family making the diet changes. Now we are stronger mental and physical watch out for us cause we will be at your local farmers market REACHING FOR THE BEETS.
I have thoroughly enjoyed this article and discussion. I am a T2D, who had gestational diabetes in my youth, with a family history of T1D. I am a health care professional, who has given instructions to diabetics using standards from ADA. I am so glad that LCHF diets are starting to be recommended. I did not ever understand why we “feed the insulin ” to treat diabetes. After proving to my MD that I have poor BG control on the recommended diet of 120 grams of carbohydrates per day, he has agreed for me to try LCHF. It is a big mindset change to allow healthy fats in my diet—at every meal!! As I research this plan of action, I would like more resources regarding T1D and LCHF. Can you make any other recommendations other than the sources mentioned above? Thanks
I’m an RN and have been mostly paleo for several years. I’ve recently been experimenting with a LCHF diet to reduce my frequent migraines, and have been reading obsessively about LCHF and keto. The information I’ve learned has impressed me to the point that I’m seriously considering a complete career change: leaving the OR to become a diabetes educator. My question: as a diabetes educator in a hospital setting, would I be allowed to teach patients how to manage their diabetes using a low-carb approach, or would I be stuck having to teach according to the arcane ADA guidelines? No way would I be OK telling a diabetic (or anyone!) to eat according to the menu you posted above! I know there are plenty of studies supporting low-carb for diabetes so I could argue my case, but I’m not sure I want to venture into a career which could be an endless series of battles.
This depends on who your boss is, but I would show evidence to back up your views and try it out on your boss and those patients who are open to eating better.
I just finished reading The South Beach Diet on a friends recommendation. I had heard about this approach to a life style diet but never considered it thinking it was just a “fad diet”. It has some pretty sensible information and I’m looking forward to giving it a try. I would be interested in hearing your thoughts, opinion on Dr. Agatston’s work.
Oh my gawsh!!! So true!!! I’m type 2 at 6.3 A1C and am off Lantus and Januvia now with weight training and nutrition training. I used A+A Wellness as my coaches. The only fructose I have is dark berries in my morning shake. The only bread I eat is flourless (coconut fl, almond fl, and arrow root) and the only pizza crust is cauliflower/cheese.
Just because it’s on the internet doesn’t mean it’s true!!!!!!!!
As a founder of a keto for glucose control focussed Facebook group, I can tell ‘out the problem isn’t just that the ‘officials’ won’t tell us the truth
The other half is patients have two main lines of thought.
I can’t give us xyz and ‘well my doctor says. . .’
In fact, we just had a members leave the group because of the conflicting info.
Didn’t ask questions. . just bowed out because the nutritionists advice was different than ours.
Until the diabetic community gets over their hang ups on foods and lose their reverence for most people wearing lab coats . . .
I am proud to say our group has both a 5 AND 4 recent club for those who get their a1c to those levels and both are added to just about every month.
In your article you used the cigarette analogy for carb consumption.
I use a fire analogy.
You don’t control a fire by throwing more gasoline on it.
You don’t avoid a car accident by keeping the gas pedal crushed to the floor.
Control the fuel
Control the fire
Avoid the accident.
Thank you for this article.
It is voices like yours that we patients need to change the status quo and shove this monster back into its cage in the closet.
Thank you.
***Slow clap….***
Oh I am so happy to have read this article! When my primary doctor said, “Sorry, but it appears you now have diabetes!” I was shocked, but I suppose not totally surprised! I started on Dec 1, 2016 to follow a low carb lifestyle of eating and by July 2017 I had brought my A1c reading from 10.9 to 5.6!! That was a pleasant surprise. It was a shock to the Dr & her office personnel. They called me to praise my efforts, and discuss how I did it. Truthfully, eating better but no real exercise. I know, I should exercise but I honestly do not like it–at all. So despite eating right my weight only dropped 22 lbs. I’d like more gone–another 40 lbs so I’m guessing it will be exercise that brings that part about. (Sad, but a reality!)
Any suggestions on better low carb eating? Currently I eat meat, eggs, butter, cream, cheese, and veggies that grow above ground. No bread, pasta, rice, or potatoes. Limited carrots.
Thank you.
I was diagnosed with Type 2 after a heart attack when I was 50. I was put on Metformin and religiously followed the recommended diet. Guess what? 6 years later I had another heart attack this time requiring a double bypass. My Metformin dosage was increased. My best friend was also type 2. He was more advanced than I was and ended up on insulin injections. He was diagnosed with sclerosis of the liver even though he was teetotal all his life. He then got an ulcer on his leg which never healed an he ended up having the leg amputated. He died a few weeks later as his organs gave up. It was a turning point for me so I started doing some research. I was determined my friend’s death would not be vain. That’s when I discovered the research regarding LCHF and went for it. After 7 weeks my blood glucose was in the normal range and I came off my medication. Whatever needs to be done to get this message out there needs to be done urgently.
I’ve been so confused on which diet to follow. I have friends who have done well on both. Most their doctors recommend the very low carb/ketosis diet. Because they are type 2 diabetic. As am I. However I came across the plant based diet and was curious as to how it really helped people.
I have 4 friends doing that diet with excellent results. But they aren’t diabetic. Just scared to do it wrong. And confused as to which is better for me. And so I am floundering.
Hey, thanks for sharing. I am looking to help myself and my husband with our blood sugar issues. Are you a very low carb dieter? Do you try to get into ketosis?
You could try both and monitor your blood glucose regularly and see which worked best for you.
Excellent article, Diana. I’ve shared it on my FB timeline. Type 2 Diabetes for some time now. I’m sure I speak for others who have problems with the rest of the family ‘not getting it’, and consequently, the pantry, refrigerator and freezer are filled up with carbohydrate/sugar rich foods. It makes it difficult (not impossible, though) to stick to a low to no carb (< = 25g ) regimen. My wife likes to go out to eat, and I'm generally stuck with a dinner salad with oil/balsamic vinaigrette dressing. Sugar is everywhere, especially the sauces on everything. Luckily, I like omelets with cheese, bacon, steak bits, etc. Thanks for the article.
I’m sorry but I have never read such a load of nonsense and generalizing.
I have been a diabetic for over 30 years and I have never been told that over-eating sugar is ‘good’.
Sugar is a carb and should be taking into account in no other way. A cooky has indeed as many carbs as a slice of bread. I sometimes eat an cooky and I feel great and have no other physical problem. The problem is overeating: sugar, others carbs that’s clear but the same goes for overeating meats or vegetables.
The way you put things it looks like the only way for a diabetic to stay alive is to stop living: only eat meat and never any kind of sugar (or other carbs)
I’m afraid you are one those people that scare other people into buying into some dietplan or, in your case, paleo. tell them they are doing everything wrong, bring up some semi-truths (which are hardly scientifically supported) and they will buy your ‘product’: paleo will save you.
Sorry I have only one conclusion: don’t fall for this bullshit.
I know this article and your comment is quite old but you missed the point of it entirely. Her point was that the advice that Nutritionists are making are often outdated and does not apply to everyone. To call this “bullshit” as you so eloquently put it, is a very myopic view. Moderation is only a way to keep people fat and happy, and a way to make people think they’re helping themselves by giving into cravings and setting themselves up for failure. You seem to think you’re very smart and sticking it to a professional that wrote a very informative article, but you’re the one who is coming off as the ignorant one.
I guess this article is bad news for vegans. Oh, nevermind, most vegans are not reading this because they are not suffering from these ailments. What a load of crap. Omg. You can’t be serios
So I’ve never been over weight, rarely had soda pop, dessert and the like, but went in to a bypass surgery non diabetic (know from pre surgical tests) and had to be treated while in recovery with insulin??!?!??
Please address my question.
T
Its 5:37pm on New Years Eve. I am not celebrating. I am sitting here in utter exhaustion. My alarm clock will be going off at 2:30am so I can make a 6am flight for my brother’s funeral. He was pronounced dead just over 24 hours ago.
What did he die of? Massive cardiac event.
What caused this event? 80% calcium buildup in his arteries and heart valves and pulmonary hypertension.
How did he come to have those conditions? According to his doctors, its the result of not the best phosphorus control while on dialysis.
Why was he on dialysis? End stage renal failure.
What caused the kidney disease? Type 2 Diabetes and blood glucose control that his endo seemed pleased with.
BTW – he was also blind due to diabetic retinopathy. He had his left foot amputated a few months ago. Poor circulation (calcium deposits again) and poor healing (high BG levels) eventually lead him to dry gangrene, extreme pain, hallucinations from being sceptic, multiple surgeries, and in the end, amputation.
He had been under near constant supervision. His diet totally out of his control. Can’t shop or cook very well when you can’t see.
But he ate regular desserts like pie because his dieticians and doctors told him he could eat anything in moderation. He had no clue how these items affected his BG levels because they insisted he not test more than once or twice a week. His endo had him using a CGM periodically but would not give him any of the data.
His A1Cs were always high. The doctors just added more medication. They actually had the gall to look me in the eye and tell me it was all inevitable, that diabetes is a progressive disease.
My brother was diagnosed almost 20 years ago. After he was diagnosed, I paid a lot more attention to my own diet. I followed similar guidelines to what he was given. Avoided fat and most meat, more whole grains, vegetable oils, lots of fruit, etc.
Just under four years ago I was diagnosed diabetic with an A1C of 10.4. Three weeks after my brother went blind. The dietician I went to told me I was in horrible shape, would end up on multiple medications, that insulin wouldn’t work because I am Type2.
If I paid attention to the majority of the medical establishment, I’d blow my brains out right now. I know exactly where that leads.
I did things differently. I insisted on testing my BG levels, especially after meals. I quickly realized that the instructions I was given were utter crap. I discovered diets like keto and paleo. I now eat no processed food with the exception of cheese and bacon. Lots of fresh vegetables and meats. No grains, beans, fruits (with exception of things like avocado, etc), most root vegetables, etc.
End result: my last A1C was 4.8. I rarely catch my BG levels over 100 and almost never above 120.
What’s to say. I am sad, angry. No, not angry. I am bloody furious. I wish these lies would stop being spread. I think the medical establishment who keeps pushing these outdated ideas would be improved by a number of good law suits, imprisonment, and end in multiple executions.
I did mention I am REALLY angry right now.
Sorry to hear that happened. Things like that make us angry too, which is one of the big reasons we do all this.
I am truly sorry for your loss.
Your fury is of course completely justified. I too have been to bad doctors — one in particular whose advice would have killed me had i followed it.
It is rare to find medical professionals who actually understand diabetes. The level of ignorance that exists is inexcusable.
I wish I had more to offer. And I wish you continued good health.
Just spent an hour reading all the comments. I was diagnosed pre-diabetic about 5 months ago and prescribed metformin low dose. It made me really sick. Constant “black oil” diarrhea and stomach pain, so I gradually stopped taking it – I was too sick to even do the follow-up blood test and doctor visit. Then I found out about a lchf diet. First stopped having sugar and then moved over to reducing carbs and bought myself a blood glucose meter and did a lot of testing. Now I know what I need to eat less of. The worst culprits are white bread hamburger buns and big plates of potato gnocchi. When I stick to lchf eating my blood sugar tests come out normal and I feel a lot better. Who knows, without the info on the internet, I’d just keep progressing to type 2 diabetes. PS. I’ve also lost a lot of weight and have not even been trying.
Thank you for this article, Diana. I was diagnosed with Type 1 diabetes 30 years ago. At the time, I met with a nutritionist who put me on the ADA diet (high carb, low fat and 5 meals a day). No fun. Gained 30 lbs and could not live with myself. I cut my calories on the same low fat diet and lost the weight, but my blood sugar was a rollercoaster. I was always to keep candy on me for emergency low blood sugars. In other words, high sugar intake. I would take insulin to chase the carbs or sugar and pass out at work, at home,in restaurants, once even behind the wheel. I joined Crossfit in 2009 and discovered the paleo diet. I tried it and after a week, I could not believe how even my blood sugar stayed. I love eating this way – I can live my life without worrying. I’ve been eating this way now ever since and now take less than half of the insulin I took years ago. I do not get hypoglycemia anymore (and I test my blood sugar a lot)! The extra fat and protein in my diet seems to keep my blood sugar stable. Diabetics (including type 1) can really benefit from a low carb diet. I never would have believed it until I tried it. It is very freeing.
Bravo Robb Wolf!! It’s a total shocker that such terrible advice is given to diabetics despite the evidence – it shocks me rigid!! The diabetes centre I attend too!! Shame on all of them!
This article is not based on SCIENCE. Stop spreading misinformation. If you read the science you’ll find that high-fat diets are associated with the development of type II diabetes. Plant-based, low fat diets are the ONLY diet that REVERSES type II diabetes. What are your recommendations based on? Because I’ve need met a patient who reversed their diabetes eating a diet rich in meats and oils.
There are numerous examples, here’s a quick one https://www.ncbi.nlm.nih.gov/pubmed/29417495 https://www.ajmc.com/focus-of-the-week/after-a-year-low-carb-diet-helps-many-patients-reverse-type-2-diabetes-lose-weight-and-stop-insulin
You, dieticians, recommend eating low fat guess what they replace the fat with sugar, I am pretty sure that people with type 2 diabetes need less sugar. Whole grains also turn into sugar. High fat does not cause diabetes because it has minimal effect on blood sugar. I was in the diabetic range and within less than a month of cutting out all carbs except from vegetables I was not. Why do all the patients who are on the recommended diabetic diet end up needing more insulin? I went to a nutritionist and I laughed at what she told me because I knew it was all wrong. I told my doctor that I would not go on medication because I can reverse it with foods because most diabetics that end up on insulin stay on it forever because of the diet nutritionists are recomending. Maybe you should watch this ted talk: https://www.youtube.com/watch?v=da1vvigy5tQ
Furthermore, the standard American diet is not a high carb diet, it’s a high fat diet. People aren’t binging on sweet potatoes, whole grain bread and brown rice, they’re eating pizza (high fat), donuts (high fat), meat (high fat), and french fries (high fat). Countries that eat a high carb diet, like the Okinawans in Japan, eat a high carb diet (90% plant foods) and have the lowest rates of chronic disease. My patients who eat low carb and high fat diets have diabetes for the rest of their life. They never reverse it.
Pizza is high carb, donuts are high carb, french fries are also high carb. Not only are they high carb or sugar, the quality of fat in those foods is bad too (high omega-6 cheap, processed oils for frying and such). Eating meat never gave anyone diabetes.
Eating higher carb whole foods (not modern processed foods) and living a good lifestyle may be healthy for some people. I won’t say that can’t be true. There have been studied hunter-gatherer people who seem to have done well on whole food higher carb diets.
It seems to be what people don’t eat (the modern processed junk) more than what they do eat.
And there are plenty of people out there reversing diabetes with low carb diets.
Amen! I have been a diabetic for 47 years. When first diagnosed, I was told not to eat anything that contained sugar. Then, I’ve watched over the years as things have changed. I figured out years ago that if I wanted my blood sugars to be in control, eating lots of vegetables, good protein and avoiding corn, wheat, potatoes, pasta…would give me the blood sugars I wanted. Thank you for writing this!!!
When any person or article uses the words ‘moderation’ or ‘balanced’, it should set off loud alarm bells and bring diwn the cone-of-scepticism. They are specifically used as psychological manipulation as they carry connotations of virtue. I mean, what kind of crackpot would you have to be to reject moderation and balance 😡?
I’m so happy I found this web site. A month ago I had routine blood work done. I got a call from the medical assistant that I was diabetic and I had to come in to discuss medication options with my doctor. I wasn’t just mad, I was livid! How do you tell a person over the phone that because of 1 blood test they’re diabetic? Also, why do I have to go on medication? Can I not control it by diet like I did before? I’m angry that a doctor would tell me that without seeing me first. Turns out my fasting was 228 which is high and I’ve had gestational diabetes but controlled it with diet alone. So when I monitored at home I was 284 the first day. Now I’m already down to 208 and lost a few pounds. I can do better of course. The next week I’m eating all paleo with intermittent fasting. The fact that I went down almost 80 pts in a couple of weeks shows me I can do this but I have to put the work in.
You are more than right here, but the problem for some of us is that the foods left on the “acceptable” list are simply unacceptable. I am expected to eat from a potential diet of foods I simply do not like…at all. The thought of slabs of meat is revolting to me. Fish is even worse. Even the list of vegetables that are acceptable is woefully thin. Type 2 diabetics have limited choices. If personal tastes matter at all, those choices can shrink to almost nil. I am convinced it is not possible to construct a diet of foods I can tolerate, let alone like. So I am down 80 lbs, and it does little to no good in terms of blood sugars. I am hungry nearly all the time. I exercise an hour daily. All for nothing. So the so-called diabetes educators lie, yes. But it’s not like anyone else has a better answer.
From your list above I guess I should be living on broccoli and butter. But that’s not a terribly compelling answer to a life problem.
I have type 2 and have been eating low carb for a bit over a year, and it’s worked well for me. It’s possible that you might have a different diabetes (maybe type 1?).
The vegetables I eat are mostly leafy greens, Chinese greens, cabbage, chiles, etc. Also tomatoes and onions, which are considered moderate-carb, but are ok if you don’t overdo it. It’s almost all “regular” food, not much exotic (except the Asian stuff… but I’m Asian) or even trendy. Even the meats are boring.
In addition to that, I eat meat and eggs. It’s around 3oz to 6oz at a time. Not that much by American standards. I also eat tofu for protein – though they are a bean, they have fewer carbs than other beans.
To be honest, it’s not that different from how I ate before the type 2 diagnosis, except that I used to eat a huge amount of bread and crackers, and could gorge on rice.
My A1C at last test was 5.2%, and I keep my BG in the 90mg/dl to 130mg/dl range most of the time. (That’s including post-meal measurements.) I sometimes exceed that. I also lost 70 lbs of weight, which sounds like a lot, but it’s not, as I had tipped over into morbid obesity.
Nothing in moderation. LOL.
I’m blogging about it here: https://complainingaboutfood.wordpress.com/
THANK YOU!
I realized my doctor was killing me so I did what I thought was right: I fired his team and eliminated all bread/grain products from my life. Although I still had sugar in my diet (I love pickeled herring) my numbers returned to normal eating fruit, vegetables, nuts, seeds, and unadulterated fish, chicken, and red meat. I eliminated all low fat products because if you read labels… low fat =added sugar and all sorts of lab chemicals. Interestingly the foods I chose to eat score low on the glycemic scales, that was coincidence as I had no knowledge of them at the time.
Once the pallette is clean you taste the salt in celery and the sugar in peas and carrots. When I watch a movie I substitute frozen peas or nuts for the popcorn or pretzels I used to have. I love infused water… Basil is my absolute favorite! I did try to go vegetarian but beans made my sugars skyrocket and I felt sick again.
Its so incredibly frustrating dealing with medical professionals who are maintaining traditional diabetes recommendations. In central Wisconsin the doctors get excited to diagnose you. When the doctor told me the news they did everything but a balloon drop and trumpets. I’m sure they saw dollar signs. The doctor then told me to “get bariatric surgery because it cures diabetes.” He tried to insist on scheduling the surgery immediately. I’m a size 14, overweight, but certainly not needing a surgery that doesn’t do what he said it would do and puts me at risk for malnutrition when I have a critical illness.
I no longer go to any doc because I’m treated horribly for not following their traditional recommendations. I need to move to a much more progressive location.
I have had type 1 for 50 years and followed the ADA recommendations for about 45 of them. Low carb and greatly improved numbers for 5 years. I would like to Sue the ADA for damages. Search for the ‘Banting level aponsors’ of the ADA. We know why we are taught to do what kills us.
Oh, I wish I knew then what I know now. 20 years ago dx gestational, went on insulin and ADA diet. Years later A1C steady ~6.5. Finally dx LADA, went VLCHP, thanks to Dr Bernstein’s Diabetes Solution and an understanding osteopath, and adjusted insulin. last 1 1/2 years, A1C 4.6-4.9 and it’s a no-brainer to maintain.
Macadamia nuts are low carb…
Just saying.
I have been a type ll diabetic since the 1970s, and my weight got out of wack. I try not to bore, as the internet is too exciting for me too. Apparently, at least for some, type ll can be beaten. The internet is full of purported solutions for type ll. I like fruit. which is indeed “sugary,” but I eat a lot of fruit since it’s supposedly “natural.” it’s quite possible an internist would just not endorse fruit eating! I am not a d.o. nor m.d. Good luck kicking desserts, pie, cake, candy and soda pop as much as you possibly can. I’m frankly worried that I eat too much fruit!
Amazing piece of content, Thanks for putting everything under one roof!